You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
CORONAVIRUS: HE KNEW; HE LIED; & at Least1,150,427 IN THE USA HAVE DIED - ((NEW VIRUS - NEW WARNINGS !!!))
- Thread starter QueEx
- Start date
U.S. records 77,000 new COVID-19 cases, blowing past previous high
The U.S. hit a new single-day record for COVID-19 infections Thursday: 77,217, by Reuters' count, and more than 75,600, according to The New York Times. The previous record, about 69,000, was set last Friday. The seven-day average of daily infections is now above 63,000, from about 22,200 a month ago. The death toll on Thursday, 969, was the highest since June 10, and Florida, Texas, and South Carolina all had their biggest one-day increases.
Other states that have broken their single-day fatality records this week are Alabama, Arizona, Hawaii, Montana, Oregon, and Utah. More than half of U.S. states now require wearing a mask in public.
Source: Reuters, The New York Times
.
The U.S. hit a new single-day record for COVID-19 infections Thursday: 77,217, by Reuters' count, and more than 75,600, according to The New York Times. The previous record, about 69,000, was set last Friday. The seven-day average of daily infections is now above 63,000, from about 22,200 a month ago. The death toll on Thursday, 969, was the highest since June 10, and Florida, Texas, and South Carolina all had their biggest one-day increases.
Other states that have broken their single-day fatality records this week are Alabama, Arizona, Hawaii, Montana, Oregon, and Utah. More than half of U.S. states now require wearing a mask in public.
Source: Reuters, The New York Times
.
Trump suggests masks are UNSAFE in off-the-rails interview
Americans Are Officially Banned From Traveling to the Bahamas Because of COVID-19
NO WAY OUT
Tom Sykes
Updated Jul. 20, 2020 6:59AM ET Published Jul. 20, 2020 6:27AM ET

HOANG DINH NAM
American tourists will be barred from entering the Bahamas starting Wednesday, as levels of COVID-19 resurge in the U.S. The situation in the Bahamas has deteriorated “at an exponential rate” since the reopening of international borders on July 1, the country’s prime minister, Hubert Minnis, said. He said the country’s national airline, Bahamasair, will cease flights to the United States, effective immediately. From Wednesday, international flights and commercial vessels carrying passengers will not be permitted to enter the borders unless they come from Canada, the United Kingdom, or the European Union. Minnis did not call out the U.S. by name, but pointedly said citizens in other countries were “ignoring health guidelines.” Florida, one of the largest tourism markets for the Bahamas, reported 12,478 new COVID-19 cases on Sunday alone.

NO WAY OUT
Tom Sykes
Updated Jul. 20, 2020 6:59AM ET Published Jul. 20, 2020 6:27AM ET
HOANG DINH NAM
American tourists will be barred from entering the Bahamas starting Wednesday, as levels of COVID-19 resurge in the U.S. The situation in the Bahamas has deteriorated “at an exponential rate” since the reopening of international borders on July 1, the country’s prime minister, Hubert Minnis, said. He said the country’s national airline, Bahamasair, will cease flights to the United States, effective immediately. From Wednesday, international flights and commercial vessels carrying passengers will not be permitted to enter the borders unless they come from Canada, the United Kingdom, or the European Union. Minnis did not call out the U.S. by name, but pointedly said citizens in other countries were “ignoring health guidelines.” Florida, one of the largest tourism markets for the Bahamas, reported 12,478 new COVID-19 cases on Sunday alone.
Americans Banned From Traveling to the Bahamas
Country’s PM closes door to visitors from the U.S. because of surge in cases, but tourists from Canada and Europe are still welcome.
www.thedailybeast.com
Florida reports more than 10,000 COVID-19 cases for 5th consecutive day
Florida recorded 12,523 new cases of COVID-19 on Saturday — the fifth day in a row the state reported more than 10,000 new infections. Rep. Donna Shalala (D-Fla.) said on Sunday's This Week there is "community spread, which means the virus is out of control." Shalala also accused Gov. Ron DeSantis (R), who will not issue a statewide mask order, of doing Floridians a disservice by pushing to reopen the state too quickly. "The residents here are terrified and I'm terrified, for the first time in my career because there's a lack of leadership," she said. On average, the United States is reporting 60,000 new COVID-19 cases a day, Reutersreports.
At least 3.7 million coronavirus cases have been recorded in the country, and the death toll has surpassed 140,000.
Source: Reuters, CNBC
Florida recorded 12,523 new cases of COVID-19 on Saturday — the fifth day in a row the state reported more than 10,000 new infections. Rep. Donna Shalala (D-Fla.) said on Sunday's This Week there is "community spread, which means the virus is out of control." Shalala also accused Gov. Ron DeSantis (R), who will not issue a statewide mask order, of doing Floridians a disservice by pushing to reopen the state too quickly. "The residents here are terrified and I'm terrified, for the first time in my career because there's a lack of leadership," she said. On average, the United States is reporting 60,000 new COVID-19 cases a day, Reutersreports.
At least 3.7 million coronavirus cases have been recorded in the country, and the death toll has surpassed 140,000.
Source: Reuters, CNBC
Three Coronavirus Vaccine Developers Report Promising Initial Results
LONDON — The race for a vaccine against the coronavirus intensified on Monday as three competing laboratories released promising results from early trials in humans.
Now comes the hard part: proving that any of the vaccines protects against the virus, and establishing how much immunity they provide — and for how long.
“What this means is that each of these vaccines is worth taking all the way through to a Phase III study,” said Dr. Peter Jay Hotez, a vaccine researcher at the Baylor College of Medicine. “That is it. All it means is ‘worth pursuing.’” Phase III trials test how well a drug works.
Two of the vaccine developers — the first, a partnership between Oxford University and the British-Swedish drug maker AstraZeneca; the second, the Chinese company CanSino Biologics — published their early results as peer-reviewed studies in The Lancet, a British medical journal.
Full Article:https://www.nytimes.com/2020/07/20/world/covid-coronavirus-vaccine.html
LONDON — The race for a vaccine against the coronavirus intensified on Monday as three competing laboratories released promising results from early trials in humans.
Now comes the hard part: proving that any of the vaccines protects against the virus, and establishing how much immunity they provide — and for how long.
“What this means is that each of these vaccines is worth taking all the way through to a Phase III study,” said Dr. Peter Jay Hotez, a vaccine researcher at the Baylor College of Medicine. “That is it. All it means is ‘worth pursuing.’” Phase III trials test how well a drug works.
Two of the vaccine developers — the first, a partnership between Oxford University and the British-Swedish drug maker AstraZeneca; the second, the Chinese company CanSino Biologics — published their early results as peer-reviewed studies in The Lancet, a British medical journal.
Full Article:https://www.nytimes.com/2020/07/20/world/covid-coronavirus-vaccine.html

"We have done it. We have done it in New York," Dr. Anthony Fauci said of how NY brought COVID-19 under control. https://7ny.tv/2WEdSnG
Dr. Fauci claps back at Trump after Trump called him an “alarmist”
MURDERER!


Dr. Fauci brilliantly claps back at Trump
DR. FAUCI RECEIVES THREATS FOR PUBLIC HEALTH ANALYSIS
DR. FAUCI RECEIVES THREATS FOR PUBLIC HEALTH ANALYSIS: Dr. Anthony Fauci speaks with the Center for Strategic and International Studies on the ongoing COVID-19 pandemic and the United States’ strategy in stopping the spread. Recently Pres. Trump has been at odds with Dr. Fauci on how the nation is handling the outbreaks, calling the country’s leading expert in infectious diseases ‘a little bit of an alarmist’ in his warnings. As Trump continues to suggest that there will be a widely available vaccine by the end of the year, Dr. Fauci believes otherwise. He told CNN yesterday ‘we could start talking about real normality again’ in 2021 when there would potentially be enough doses for tens of millions of people. Fauci also mentioned how he has recently been given a security detail due to some ‘hate mail and serious threats,’ which he responded to by saying ‘as much as people inappropriately, I think, make me somewhat of a hero— and I'm not a hero, I'm just doing my job— there are people who get really angry at thinking I'm interfering with their life because I'm pushing a public-health agenda.'
DR. FAUCI RECEIVES THREATS FOR PUBLIC HEALTH ANALYSIS: Dr. Anthony Fauci speaks with the Center for Strategic and International Studies on the ongoing COVID-19 pandemic and the United States’ strategy in stopping the spread. Recently Pres. Trump has been at odds with Dr. Fauci on how the nation is handling the outbreaks, calling the country’s leading expert in infectious diseases ‘a little bit of an alarmist’ in his warnings. As Trump continues to suggest that there will be a widely available vaccine by the end of the year, Dr. Fauci believes otherwise. He told CNN yesterday ‘we could start talking about real normality again’ in 2021 when there would potentially be enough doses for tens of millions of people. Fauci also mentioned how he has recently been given a security detail due to some ‘hate mail and serious threats,’ which he responded to by saying ‘as much as people inappropriately, I think, make me somewhat of a hero— and I'm not a hero, I'm just doing my job— there are people who get really angry at thinking I'm interfering with their life because I'm pushing a public-health agenda.'

How the mask became a symbol of white fear and Black threat
Amid the coronavirus crisis, many Black Americans fear that wearing a protective mask could make them a target
 www.middleeasteye.net
www.middleeasteye.net

How the mask became a symbol of white fear and Black threat
Amid the coronavirus crisis, many Black Americans fear that wearing a protective mask could make them a target
As if African Americans have not endured enough in their long and cruel history in the Unites States, during the current pandemic, they have to make yet another punishing choice.
Consider the following: the US today is one of the epicentres of the coronavirus pandemic, where public health authorities fear new cases could reach 100,000 a day. The same public health officials recommend social distancing and wearing masks when people go for a quick outing.
That is a fairly modest, yet vital, recommendation to control this disease. So when going out, many people wear masks - except if they are Black, brown, or any other colour, white people have designated this mask wearing as codification for exercising power and privilege over them. In such cases, wearing a mask has become dangerous to their wellbeing.
During the last few months, since Covid-19 started wreaking havoc in this country, we have seen instances where Black people have done what everyone is asked to do - namely, wearing masks when going out. But they have been approached by security forces and told to take their masks off for “security reasons”.
Two Black men, for example, recently reported that they were kicked out of Walmart for wearing protective masks. A Washington Post report on the incident notes that other African Americans worry about a similar fate if they do as public health officials tell them to do.
The incident is not an isolated case, as another report notes: “When the [Centers for Disease Control and Prevention] issued guidelines in early March asking people to wear masks to prevent the spread of coronavirus, the question for many Black men was not where to get a mask or which kind. It was: how do I cover my face and not get shot?”
The result is clear: “Despite their fears of infection, and statistics showing Black communities are among the hardest hit, many Black men feel wearing a mask is a bigger threat than the coronavirus.”
A further study concluded that racists who fear Black people just for being who they are “were much likelier to perceive a young Black man as threatening or untrustworthy if he was wearing a homemade mask or a bandanna, compared to a white man around the same age”.
So if they don’t wear masks, Black people are in danger of catching the virus or spreading it to others, and are thus admonished for not following public health mandates. But if they do wear them, they are subject to harassment, abuse and potentially fatal violence. So what is a Black person to do - to wear or not to wear a mask?
Downward gaze of the coloniser
In his classic masterpiece, Black Skin, White Masks, the Martiniquan revolutionary psychiatrist Frantz Fanon theorised his own experiences as a Black man reacting to the dehumanising effects of racism and colonialism. In this seminal text, Fanon narrows in on the brutal violence inherent in the downward gaze of the coloniser dismantling the colonised person’s sense of selfhood. The power and self-universalisation of colonial institutions are thus internalised by the Black person to the point of self-hatred.
About a decade after Fanon, Malcolm X also articulated this self-hatred. In a May 1962 speech in Los Angeles, he wondered: “Who taught you to hate the texture of your hair? Who taught you to hate the colour of your skin to such extent that you bleach to get like the white man? Who taught you to hate the shape of your nose and the shape of your lips? Who taught you to hate yourself from the top of your head to the soles of your feet? Who taught you to hate your own kind?”

Police arrest a man at Black Lives Matter Plaza in Washington on 4 July
Between Fanon in 1950s and Malcolm X in 1960s, the internalised colonial gaze was effectively exposed, articulated and theorised, so that subsequent generations of the struggle for justice would de-mythologise and dismantle the downcast gaze of the colonial power.
Half a century later, in my Brown Skin, White Masks, I carried Fanon’s and Malcolm X’s insights further and brought them to our own time, thinking through the ways in which native informers from the Arab and Muslim world aid and abet US imperial projects, precisely because of this self-hatred and full identification with the ruling white supremacy.
I argued that a critical reading of the exiled intellectual Edward Said had a darker side, which dwelled in expatriate Arab and Muslim intellectuals putting their services at work for the ruling dysfunctional empire.
Further advancing the argument, in his Red Skin, White Masks: Rejecting the Colonial Politics of Recognition, Glen Sean Coulthard also challenged the rubric of “recognition” as a modus operandi of identity politics in a kind of liberalism that seeks to whitewash the colonial atrocities of settler-colonialism against indigenous people.
Empty white masks
From Fanon forward, therefore, we have a sustained course of critical insights articulating the psychopathology of the relation between faces and masks in internalised colonial contexts. People are conditioned to hate their own physical truth and to denounce their own parental heritage by way of facilitating a meagre existence in this quintessentially racist world.
Today, these inaugural insights of Fanon and others have reached a turning point, where embedded in the Black Lives Matter uprising in the US and around the world is the pride of place and dignity of one’s own face and features behind any masks, which now have purely practical purposes, as recommended by public health officials.
The struggle of Black Lives Matter is now geared towards a moment when Black, brown or any other colonially manufactured “coloured” people wear their medically recommended masks, liberated from the false consciousness of identifying with their self-designated white masters.
As the statues of European and American racist icons crumble on both sides of the Atlantic, masks have overcome their racist metaphoric sense and become entirely pragmatic.
Paradoxically, however, masks have assumed an entirely different symbolic meaning today - this time for self-designated “white people”, where the racist followers of US President Donald Trump have turned not wearing masks into a political declaration of their ignorant defiance of public health recommendations.
Their existence is so solidly based on their “white face” that wearing a mask would deny and destroy the very essence of their selfhood. Their white faces have turned into empty masks of their soulless selves, in search of others to define them.
Precisely at this moment, the proud and confident face of Malcolm X, decades after his tragic death, shines sharper than ever, exposing his face as the singular site of our collective, defiant, happy and confident consciousness.
The Censorship of Inequality in the Covid-19 Era: How Corporate and Market-Based Metrics Rule the News, and Why it Matters
By Anthony DiMaggio
 www.projectcensored.org
www.projectcensored.org

The Censorship of Inequality in the Covid-19 Era: How Corporate and Market-Based Metrics Rule the News, and Why it Matters
The old adage that “the more things change the more they stay the same” seems particularly appropriate to media coverage in the Covid-19 crisis. Old patterns of media bias have continued, albeit in an intensified form, as pandemic’s effects have intensified over time. Of particular concern are longstanding problems with mass media reporting, as related to the marginalization of inequality coverage during a time of rising economic instability and collapse.
News reporting has long downplayed the problem of record inequality in the U.S. In researching my forthcoming book, Unequal America, I documented how, across television, print, online, and local news, U.S. economic coverage in the 2000s and 2010s consistently emphasized market-based economic metrics – primarily of interest to corporations such as unemployment – while suppressing reporting of societal class divisions and inequality. Utilizing the Nexis-Uni historical news archive, I show how coverage of unemployment dominated the news throughout these two decades, receiving between four to five times as much coverage as inequality in the period prior to the 2008 economic crash. That imbalance continued post-2008 and into the 2010s, with unemployment receiving from five to seven times as much coverage as inequality.
The pattern of marginalizing inequality continued during the periods immediately preceding and following the onset of the Covid-19 crisis in early 2020. My examination of print, television, and local media coverage in Unequal America demonstrates that reporting on inequality fell by between a third to two-thirds from the pre-Covid period (January and March), compared to after its emergence in the U.S. (by March). Throughout this three-month period, unemployment reporting increased by two to four times, depending on the outlet I examined. By March, unemployment coverage was receiving between two to six times as much coverage per month, compared to reporting on inequality.
Unemployment remains a highly salient issue in the Covid-19 era. We face a rapid rise in jobless claims, with various estimates suggesting unemployment reached between 16 to 20 percent by late April. But it is not clear why it unemployment should be seen as a more important economic metric than inequality, at a time when Covid-19 is disproportionately ravaging neighborhoods populated by poor people of color, and low-pay service workers on the frontlines of the crisis. Racial and economic stratification remain at the center of the radically different Covid-19-related health outcomes Americans experience, when comparing poor people and poor people of color clustered together in inner city communities that are marked by extensive contacts, and more affluent white neighborhoods, with residents who benefit from greater social distancing as a result of living in less dense, sprawling suburbs.
Inequality is also highly significant when considering that lower income Americans are more likely to work in jobs that require extensive contacts between individuals, whereas higher-income white collar workers have been able to escape regular contacts with others by retreating into remote work tele-jobs that radically reduce their potential contacts with Covid-19-positive individuals. In sum, inequality remains an incredibly important metric for understanding how people have experienced this pandemic.
Despite the importance to understanding Covid-19, there has been relatively little interest in the subject, relative to journalists’ fixation on market-based economic metrics like unemployment. I learned this the hard way as a social scientist who sought to raise attention to the issue of inequality – more specifically in my failed efforts to draw reporters’ attention to the question of inequality’s relevance to Covid-19. In my exhaustive search for polling data on public opinion of the inequality question in the Covid-19 era, I was unable to identify a single national survey done in March or April addressing the inequality issue, at all, or as it relates to American politics and policy, and the potential role of government in addressing the problem of rising inequality.
I sought to rectify this hole in our understanding of Covid-19 by designing some national polling questions that covered these issues, which were then administered by the Harris Polling group. My questions, which were fielded to a nationally-representative audience in early April, revealed the following about Americans’ political-economic attitudes:
– An overwhelming 78 percent of Americans agreed that,“considering the spread of coronavirus in the U.S. and its impact on the economy and the American people,” it is “somewhat” or “very important” that “the U.S. government commit to reducing economic inequality,” over the next year, through “raising the minimum wage” and “taxing households making more than $250,000 a year to guarantee health care coverage to all American who lack access.” Only 21 percent felt reducing inequality through such actions is “not very important” or “not at all important.”
– A significant majority – 57 percent of Americans – agreed that, “in a time of growing economic instability and rising unemployment claims, the U.S. is increasingly divided between the ‘haves’ and the ‘have-nots.’”
But none of the above findings have made their way into mass media reporting, as they’ve been ignored by all the major corporations that control the news in the U.S. The school where I am employed, Lehigh University, makes serious efforts via its public relations department to promote the academic works of scholars, by sending out press releases and submitting relevant commentary and analysis pieces to their many contacts in the U.S. mass media. In my case, the press release, and an accompanying analysis piece including the information on my Harris survey results, were both sent to numerous media outlets and news aggregators commonly used by corporate media journalists to construct their news stories. My phone and email contacts were also included in the press releases, for those journalists who might choose to write a news story on public opinion of inequality in the Covid-19 era. The press release and accompanying analysis received no interest whatsoever, not from a single mainstream corporate journalist or news organization, or from any mainstream news websites that run analysis pieces on American political and economic affairs. The issue of public opinion on inequality in the Covid-19 era has been, for all intents and purposes, a non-issue – subject to a complete media blackout.
Coverage of Covid-19-related issues has understandably filled the vast majority of the news hole across mainstream news organizations, when looking at media coverage over the last few months. But what is lost in the single-minded emphasis on market-based metrics like unemployment, at the expense of inequality coverage? Importantly, we lose context in terms of understanding the variety of ways in which this pandemic has affected the economic lives of Americans. Clearly, Americans believe that inequality is an important problem that should be addressed, discussed, and deliberated upon, to assess what the public’s and the government’s responsibilities are to fellow Americans, and to those who are the most at risk, financially and health-wise, in this crisis period. But without sustained coverage of inequality’s place in the Covid-19 crisis, and without any journalistic attention to American public opinion on the inequality problem, it is unlikely that a serious discussion of what government can do to combat rising economic insecurity will happen any time soon.
"If you are waiting for Pres. Trump to use the federal government with all of its power and influence, do not, because it is not happening," warns Chris Cuomo. https://cnn.it/2P0BFdn
U.S. coronavirus death toll surpasses 150,000
The United States coronavirus death toll surpassed 150,000 Wednesday, data collected by Johns Hopkins University shows. Florida on Wednesday reported 216 new coronavirus deaths in the last 24 hours, the state's biggest one-day increase yet. Texas meanwhile added 8,324 new cases on Tuesday and 164 new deaths.
It is close to surpassing 400,000 total cases, as California, Florida, and New York already have. Spiking infections, hospitalizations, and deaths across the South and West have prompted states to halt or reverse the reopening of their economies. Federal officials released a report that found 21 states are experiencing outbreaks that put them in the "red zone." Another 28 states are in the "yellow zone," while just one, Vermont, qualified for the "green zone."
Source: Orlando Sentinel, The New York Times
.
The United States coronavirus death toll surpassed 150,000 Wednesday, data collected by Johns Hopkins University shows. Florida on Wednesday reported 216 new coronavirus deaths in the last 24 hours, the state's biggest one-day increase yet. Texas meanwhile added 8,324 new cases on Tuesday and 164 new deaths.
It is close to surpassing 400,000 total cases, as California, Florida, and New York already have. Spiking infections, hospitalizations, and deaths across the South and West have prompted states to halt or reverse the reopening of their economies. Federal officials released a report that found 21 states are experiencing outbreaks that put them in the "red zone." Another 28 states are in the "yellow zone," while just one, Vermont, qualified for the "green zone."
Source: Orlando Sentinel, The New York Times
.
Herman Cain dies from coronavirus
By Karl de Vries
and Veronica Stracqualursi,
CNN
July 30, 2020

Washington (CNN)Herman Cain, a onetime Republican presidential candidate and former CEO of Godfather's Pizza, has died from coronavirus, according to an obituary sent from his verified Twitter account and Newsmax, where he was launching a television show.
Cain, 74, was hospitalized earlier this month, and his Twitter account said earlier this week he was being treated with oxygen in his lungs. It is unknown where Cain contracted the virus.
As a co-chair of Black Voices for Trump, Cain was one of the surrogates at President Donald Trump's June 20 rally in Tulsa, Oklahoma -- which saw at least eight Trump advance team staffers in attendance test positive for coronavirus. Trump campaign spokesman Tim Murtaugh has told CNN that Cain did not meet with Trump at the Tulsa rally.
Cain announced his candidacy for president in 2011. He briefly gained traction in the race for his 9-9-9 tax reform plan, which would have replaced almost all current taxes with a 9% income tax, a 9% corporate tax and a 9% national sales tax. After about seven months, he dropped his bid for the GOP nomination amid sexual harassment allegations, which he denied.
By Karl de Vries
and Veronica Stracqualursi,
CNN
July 30, 2020

Washington (CNN)Herman Cain, a onetime Republican presidential candidate and former CEO of Godfather's Pizza, has died from coronavirus, according to an obituary sent from his verified Twitter account and Newsmax, where he was launching a television show.
Cain, 74, was hospitalized earlier this month, and his Twitter account said earlier this week he was being treated with oxygen in his lungs. It is unknown where Cain contracted the virus.
As a co-chair of Black Voices for Trump, Cain was one of the surrogates at President Donald Trump's June 20 rally in Tulsa, Oklahoma -- which saw at least eight Trump advance team staffers in attendance test positive for coronavirus. Trump campaign spokesman Tim Murtaugh has told CNN that Cain did not meet with Trump at the Tulsa rally.
Cain announced his candidacy for president in 2011. He briefly gained traction in the race for his 9-9-9 tax reform plan, which would have replaced almost all current taxes with a 9% income tax, a 9% corporate tax and a 9% national sales tax. After about seven months, he dropped his bid for the GOP nomination amid sexual harassment allegations, which he denied.
Trump on Covid death toll: 'It is what it is'

By Devan Cole, CNN
Updated 9:12 AM ET, Tue August 4, 2020
Washington (CNN)President Donald Trump said the United States' staggering death toll from coronavirus "is what it is" in a new interview, again giving his administration credit for its response despite ongoing surges in new cases and a human toll that far outpaces that of any other nation.
When confronted with the US' daily death toll and Trump's messaging on the pandemic during an interview with Axios that aired Monday night, the President grew defensive and appeared frustrated by Jonathan Swan's questions about the crisis.
"I've gone to your rallies. I've talked to your people. They love you. They listen to you. They listen to every word you say. They hang on your every word," Swan said. "And so when they hear you say, 'everything's under control. Don't worry about wearing masks,' I mean, these are people -- many of them are older people."

Trump spinning virus failure as a win again by celebrating 'encouraging' progress
Trump replied, adding: "I think it's under control."
"They are dying. That's true.
And you -- it is what it is," Trump said emphatically. "But that doesn't mean we aren't doing everything we can. It's under control as much as you can control it."
Trump has frequently defended his administration's performance to the pandemic but rarely expresses grief for the victims. When the US surged past 100,000 confirmed deaths in late May -- after weeks of Trump projecting a toll well short of that mark -- the President declined to make a public statement until the next day, tweeting about the victims amid a morning tweetstorm of insults and grievances.
When pressed on the US death toll in the Axios interview, Trump repeatedly pointed to the proportion of deaths to confirmed coronavirus cases, rather than the proportion of deaths to the US population, a figure that is arguably more telling of the state of the pandemic in the country given that the US has less than 5% of the world's population but around 25% of global deaths from Covid-19.
"Well, right here, United States is lowest in numerous categories. We're lower than the world, we're lower than Europe," Trump said as he sorted through pages of charts, handing one to Swan. "Take a look, right here -- here's case death."
"Oh, you're doing death as a proportion of cases. I'm talking about death as a proportion of population. That's where the US Is really bad," Swan said.
"You can't do that ... you have to go by the cases. The cases of death," Trump argued.
"It's surely a relevant statistic to say if the US has X population and X percentage of death of that population, versus South Korea," Swan later said, to which Trump replied: "No, because you have to go by the cases."
To the contrary, officials on the White House coronavirus task force have been warning that the pandemic is worsening in the US. On Sunday, Dr. Deborah Birx, the response coordinator for the group, said that the US is in a new phase of the pandemic where the virus "is extraordinarily widespread." Trump replied on Monday, calling Birx "pathetic."
More than 155,000 Americans are known to have died from the virus, and the death toll is projected to reach 173,000 by August 22, according to a new composite forecast from the US Centers for Disease Control and Prevention. That's an average of almost 1,000 US deaths every day for the next 30 days.
CNN's Stephen Collinson, Christina Maxouris, Holly Yan and Dakin Andone contributed to this report.

By Devan Cole, CNN
Updated 9:12 AM ET, Tue August 4, 2020
https://ht.cdn.turner.com/cnn/big/ads/advertiser/2014/2014/05/CNN_plated_logo_05_13_3sec.256x144.mp4
Trump brings his own charts to interview on Covid-19 deaths 04:55Washington (CNN)President Donald Trump said the United States' staggering death toll from coronavirus "is what it is" in a new interview, again giving his administration credit for its response despite ongoing surges in new cases and a human toll that far outpaces that of any other nation.
When confronted with the US' daily death toll and Trump's messaging on the pandemic during an interview with Axios that aired Monday night, the President grew defensive and appeared frustrated by Jonathan Swan's questions about the crisis.
"I've gone to your rallies. I've talked to your people. They love you. They listen to you. They listen to every word you say. They hang on your every word," Swan said. "And so when they hear you say, 'everything's under control. Don't worry about wearing masks,' I mean, these are people -- many of them are older people."

Trump spinning virus failure as a win again by celebrating 'encouraging' progress
"Well, what's your definition of control?"
Trump replied, adding: "I think it's under control."
"How? A thousand Americans are dying a day," Swan said.
"They are dying. That's true.
And you -- it is what it is," Trump said emphatically. "But that doesn't mean we aren't doing everything we can. It's under control as much as you can control it."
Trump has frequently defended his administration's performance to the pandemic but rarely expresses grief for the victims. When the US surged past 100,000 confirmed deaths in late May -- after weeks of Trump projecting a toll well short of that mark -- the President declined to make a public statement until the next day, tweeting about the victims amid a morning tweetstorm of insults and grievances.
When pressed on the US death toll in the Axios interview, Trump repeatedly pointed to the proportion of deaths to confirmed coronavirus cases, rather than the proportion of deaths to the US population, a figure that is arguably more telling of the state of the pandemic in the country given that the US has less than 5% of the world's population but around 25% of global deaths from Covid-19.
"Well, right here, United States is lowest in numerous categories. We're lower than the world, we're lower than Europe," Trump said as he sorted through pages of charts, handing one to Swan. "Take a look, right here -- here's case death."
"Oh, you're doing death as a proportion of cases. I'm talking about death as a proportion of population. That's where the US Is really bad," Swan said.
"You can't do that ... you have to go by the cases. The cases of death," Trump argued.
"It's surely a relevant statistic to say if the US has X population and X percentage of death of that population, versus South Korea," Swan later said, to which Trump replied: "No, because you have to go by the cases."
To the contrary, officials on the White House coronavirus task force have been warning that the pandemic is worsening in the US. On Sunday, Dr. Deborah Birx, the response coordinator for the group, said that the US is in a new phase of the pandemic where the virus "is extraordinarily widespread." Trump replied on Monday, calling Birx "pathetic."
More than 155,000 Americans are known to have died from the virus, and the death toll is projected to reach 173,000 by August 22, according to a new composite forecast from the US Centers for Disease Control and Prevention. That's an average of almost 1,000 US deaths every day for the next 30 days.
CNN's Stephen Collinson, Christina Maxouris, Holly Yan and Dakin Andone contributed to this report.
Trump on Covid death toll: 'It is what it is'
And November 3rd 2020 - Is What It Is. Remember: VOTE!!!
I am not going to stop calling out [Pres. Trump's] inaction, his lies, and his hypocrisy, because it's making us sick and it's putting our kids behind," says Chris Cuomo.
https://cnn.it/2DFj04e
https://cnn.it/2DFj04e
Forty percent of people with coronavirus infections have no symptoms. Might they be the key to ending the pandemic?
http://a.msn.com/05/en-us/BB17JpdS?ocid=sf
When researcher Monica Gandhi began digging deeper into outbreaks of the novel coronavirus, she was struck by the extraordinarily high number of infected people who had no symptoms.

© Saudi Press Agency/Via Reuters Muslim pilgrims wearing face masks and keeping social distance last week during the annual Haj
pilgrimage in Mecca.
A Boston homeless shelter had 147 infected residents, but 88 percent had no symptoms even though they shared their living space.
A Tyson Foods poultry plant in Springdale, Ark., had 481 infections, and 95 percent were asymptomatic.
Prisons in Arkansas, North Carolina, Ohio and Virginia counted 3,277 infected people, but 96 percent were asymptomatic.
During its seven-month global rampage, the coronavirus has claimed more than 700,000 lives. But Gandhi began to think the bigger mystery might be why it has left so many more practically unscathed.
What was it about these asymptomatic people, who lived or worked so closely to others who fell severely ill, she wondered, that protected them? Did the “dose” of their viral exposure make a difference? Was it genetics? Or might some people already have partial resistance to the virus, contrary to our initial understanding?
Efforts to understand the diversity in the illness are finally beginning to yield results, raising hope the knowledge will help accelerate development of vaccines and therapies — or possibly even create new pathways toward herd immunity in which enough of the population develops a mild version of the virus that they block further spread and the pandemic ends.
“A high rate of asymptomatic infection is a good thing,” said Gandhi, an infectious-disease specialist at the University of California at San Francisco. “It’s a good thing for the individual and a good thing for society.”
The coronavirus has left numerous clues — the uneven transmission in different parts of the world, the mostly mild impact on children. Perhaps most tantalizing is the unusually large proportion of infected people with no symptoms. The Centers for Disease Control and Prevention last month estimated that rate at about 40 percent.
Those clues have sent scientists off in different directions: Some are looking into the role of the receptor cells, which the virus uses to infiltrate the body, to better understand the role that age and genetics might play. Others are delving into face masks and whether they may filter just enough of the virus so that those wearing them had mild cases or no symptoms at all.
The theory that has generated the most excitement in recent weeks is that some people walking among us might already have partial immunity.
https://web.whatsapp.com/send?text=http://a.msn.com/05/en-us/BB17JpdS?ocid=sw
When SARS-CoV-2 was first identified on Dec. 31, 2019, public health officials deemed it a “novel” virus because it was the first time it had been seen in humans who presumably had no immunity from it whatsoever. There’s now some very early, tentative evidence suggesting that assumption might have been wrong.
One mind-blowing hypothesis — bolstered by a flurry of recent studies — is that a segment of the world’s population may have partial protection thanks to “memory” T cells, the part of our immune system trained to recognize specific invaders. This could originate from cross protection derived from standard childhood vaccinations. Or, as a paper published Tuesday in Science suggested, it could trace back to previous encounters with other coronaviruses, such as those that cause the common cold.
“This might potentially explain why some people seem to fend off the virus and may be less susceptible to becoming severely ill,” National Institutes of Health Director Francis Collins remarked in a blog post this past week.
On a population level, such findings, if validated, could be far-reaching.
Hans-Gustaf Ljunggren, a researcher at Sweden’s Karolinska Institute, and others have suggested that public immunity to the coronavirus could be significantly higher than what has been suggested by serology studies. In communities in Boston, Barcelona, Wuhan and other major cities, the proportion of people estimated to have antibodies and therefore presumably be immune has mostly been in the single digits. But if others had partial protection from T cells, that would raise a community’s immunity level much higher.
This, Ljunggren said, would be “very good news from a public health perspective.”
Some experts have gone so far as to speculate whether some surprising recent trends in the epidemiology of the coronavirus — the drop in infection rates in Sweden where there have been no widespread lockdowns or mask requirements, or the high rates of infection in Mumbai’s poor areas but little serious disease — might be due to preexisting immunity.
Others say it’s far too early to draw such conclusions. Anthony S. Fauci, the United States’ top infectious-disease expert, said in an interview that while these ideas are being intensely studied, such theories are premature. He agreed that at least some partial preexisting immunity in some individuals seems a possibility.
And he said the amount of virus someone is exposed to — called the inoculum — “is almost certainly an important and likely factor” based on what we know about other viruses.
But Fauci cautioned there are multiple likely reasons — including youth and general health — that determine whether a particular individual shrugs off the disease or dies of it. He also emphasized that even those with mild illness may have lingering medical issues.
That reinforces the need, in his view, for continued vigilance in social distancing, masking and other precautions.
“There are so many other unknown factors that maybe determine why someone gets an asymptomatic infection,” Fauci said. “It’s a very difficult problem to pinpoint one thing.”
Immune memory machine
News headlines have touted the idea based on blood tests that 20 percent of some New York communities might be immune, 7.3 percent in Stockholm, 7.1 percent in Barcelona. Those numbers come from looking at antibodies in people’s blood that typically develop after they are exposed to a virus. But scientists believe another part of our immune system — T cells, a type of white blood cell that orchestrates the entire immune system — could be even more important in fighting against the coronavirus.
Recent studies have suggested that antibodies from the coronavirus seem to stick around for only two to three months in some people. While work on T cells and the coronavirus is only getting started — testing T cells is much more laborious than antibody testing — previous research has shown that, in general, T cells tend to last years longer.
One of the first peer-reviewed studies on the coronavirus and T cells was published in mid-May in the journal Cell by Alessandro Sette, Shane Crotty and others at the La Jolla Institute for Immunology near San Diego.
The group was researching blood from people who were recovering from coronavirus infections and wanted to compare that to samples from uninfected controls who were donors to a blood bank from 2015 to 2018. The researchers were floored to find that in 40 to 60 percent of the old samples, the T cells seemed to recognize SARS-CoV-2.
“The virus didn’t even exist back then, so to have this immune response was remarkable,” Sette said.
Research teams from five other locations reported similar findings. In a study from the Netherlands, T cells reacted to the virus in 20 percent of the samples. In Germany, 34 percent. In Singapore, 50 percent.
The different teams hypothesized this could be due to previous exposure to similar pathogens. Perhaps fortuitously, SARS-CoV-2 is part of a large family of viruses. Two of them — SARS and MERS — are deadly and led to relatively brief and contained outbreaks. Four other coronavirus variants, which cause the common cold, circulate widely each year but typically result in only mild symptoms. Sette calls them the “less-evil cousins of SARS-CoV-2.”
This week, Sette and others from the team reported new research in Science providing evidence the T cell responses may derive in part from memory of “common cold” coronaviruses.
“The immune system is basically a memory machine,” he said. “It remembers and fights back stronger.”
Interestingly, the researchers noted in their paper, the strongest reaction they saw was against the spike proteins that the virus uses to gain access to cells — suggesting that fewer viral copies get past these defenses.
“The current model assumes you are either protected or you are not — that it’s a yes or no thing,” Sette added. “But if some people have some level of preexisting immunity, that may suggest it’s not a switch but more continuous.”
Childhood vaccines
 A scientific illustration of the SARS-CoV-2 coronavirus binding to a receptor on a human cell. This attachment is the initial step in the development of a coronavirus infection. (Kateryna Kon/Science Photo/Getty Images)
A scientific illustration of the SARS-CoV-2 coronavirus binding to a receptor on a human cell. This attachment is the initial step in the development of a coronavirus infection. (Kateryna Kon/Science Photo/Getty Images)
Nearly 2,000 miles away, at the Mayo Clinic in Rochester, Minn., Andrew Badley was zeroing in the possible protective effects of vaccines.
Teaming up with data experts from nference, a company that manages their clinical data, he and other scientists looked at records from 137,037 patients treated at the health system to look for relationships between vaccinations and coronavirus infection.
They knew that the vaccine for smallpox, for example, had been shown to protect against measles and whooping cough. Today, a number of existing vaccines are being studied to see if any might offer cross-protection against SARS-CoV-2.
The results were intriguing: Seven types of vaccines given one, two or five years in the past were associated with having a lower rate of infection with the new coronavirus. Two vaccines in particular seemed to show stronger links: People who got a pneumonia vaccine in the recent past appeared to have a 28 percent reduction in coronavirus risk. Those who got polio vaccines had a 43 percent reduction in risk.
Venky Soundararajan, chief scientific officer of nference, remembers when he first saw how large the reduction appeared to be, he immediately picked up his phone and called Badley: “I said, ‘Is this even possible?’”
The team looked at dozens of other possible explanations for the difference. They adjusted for geographic incidence of the coronavirus, demographics, comorbidities, even whether people had had mammograms or colonoscopies under the assumption that people who got preventive care might be more apt to social distance. But the risk reduction still remained large.
“This surprised us completely,” Soundararajan recalled. “Going in we didn’t expect anything or maybe one or two vaccines showing modest levels of protection.”
The study is only observational and cannot show a causal link by design, but Mayo researchers are looking at a way to quantify the activity of these vaccines on the coronavirus to serve as a benchmark to the new vaccines being created by companies such as Moderna. If existing vaccines appear as protective as new ones under development, he said, they could change the world’s whole vaccine strategy.
Genetics and biology
Click to expand
The novel coronavirus is a master of disguise: Here's how it works
At NIH headquarters in Bethesda, Md., meanwhile, Alkis Togias has been laser-focused on one group of the mildly impacted: children. He wondered if it might have something to do with the receptor known as ACE2, through which the virus hitchhikes into the body.
In healthy people, the ACE2 receptors perform the important function of keeping blood pressure stable. The novel coronavirus latches itself to ACE2, where it replicates. Pharmaceutical companies are trying to figure out how to minimize the receptors or to trick the virus into attaching itself to a drug so it doesn’t replicate and travel throughout the body.
Was it possible, Togias asked, that children naturally expressed the receptor in a way that makes them less vulnerable to infection?
He said recent papers have produced counterintuitive findings about one subgroup of children — those with a lot of allergies and asthma. The ACE2 receptors in those children were diminished, and when they were exposed to an allergen such as cat hair, the receptors were further reduced. Those findings, combined with data from hospitals showing that asthma did not seem to be a risk factor for the respiratory virus, as expected, have intrigued researchers.
“We are thinking allergic reactions may protect you by down-regulating the receptor,” he said. “It’s only a theory of course.”
Togias, who is in charge of airway biology for the National Institute of Allergy and Infectious Diseases, is looking at how those receptors seem to be expressed differently as people age, as part of a study of 2,000 U.S. families. By comparing those differences and immune responses within families, they hope to be able to better understand the receptors’ role.
Separately, a number of genetic studies show variations in genes associated with ACE2 with people from certain geographic areas, such as Italy and parts of Asia, having distinct mutations. No one knows what significance, if any, these differences have on infection, but it’s an active area of discussion in the scientific community.
Masks
 A passenger in quarantine February on the Diamond Princess cruise ship in Yokohama, Japan. (Takashi Aoyama/Getty Images)
A passenger in quarantine February on the Diamond Princess cruise ship in Yokohama, Japan. (Takashi Aoyama/Getty Images)
Before the pandemic, Gandhi, the University of California researcher, specialized in HIV. But like other infectious-disease experts these days, she has spent many of her waking hours thinking about the coronavirus. And in scrutinizing the data on outbreaks one day, she noticed what might be a pattern: People were wearing masks in the settings with the highest percentage of asymptomatic cases.
The numbers on two cruise ships were especially striking. In the Diamond Princess, where masks weren’t used and the virus was likely to have roamed free, 47 percent of those tested were asymptomatic. But in the Antarctic-bound Argentine cruise ship, where an outbreak hit in mid-March and surgical masks were given to all passengers and N95 masks to the crew, 81 percent were asymptomatic.
Similarly high rates of asymptomatic infection were documented at a pediatric dialysis unit in Indiana, a seafood plant in Oregon and a hair salon in Missouri, all of which used masks. Gandhi was also intrigued by countries such as Singapore, Vietnam and the Czech Republic that had population-level masking.
“They got cases,” she noted, “but fewer deaths.”
The scientific literature on viral dose goes back to around 1938 when scientists began to find evidence that being exposed to one copy of a virus is more easily overcome than being exposed to a billion copies. Researchers refer to the infectious dose as ID50 — or the dose at which 50 percent of the population would become infected.
While we don’t know what that level might be for the coronavirus (it would be unethical to expose humans in this way), previous work on other nonlethal viruses showed that people tend to get less sick with lower doses and more sick with higher doses. A study published in late May involving hamsters, masks and SARS-CoV-2 found those given coverings had milder cases than those who did not get them.
In an article published this month in the Journal of General Internal Medicine, Gandhi noted that in some outbreaks early in the pandemic in which most people did not wear masks, 15 percent of the infected were asymptomatic. But later on, when people began wearing masks, the rate of asymptomatic people was 40 to 45 percent.
She said the evidence points to masks not just protecting others — as U.S. health officials emphasize — but protecting the wearer as well. Gandhi makes the controversial argument that while we’ve mostly talked about asymptomatic infections as terrifying due to how people can spread the virus unwittingly, it could end up being a good thing.
“It is an intriguing hypothesis that asymptomatic infection triggering immunity may lead us to get more population-level immunity,” Gandhi said. “That itself will limit spread.”
coronavirus-infections-have-no-symptoms-might-they-be-the-key-to-ending-the-pandemic/ar-BB17JpdS?ocid=sf
http://a.msn.com/05/en-us/BB17JpdS?ocid=sf
When researcher Monica Gandhi began digging deeper into outbreaks of the novel coronavirus, she was struck by the extraordinarily high number of infected people who had no symptoms.

© Saudi Press Agency/Via Reuters Muslim pilgrims wearing face masks and keeping social distance last week during the annual Haj
pilgrimage in Mecca.
A Boston homeless shelter had 147 infected residents, but 88 percent had no symptoms even though they shared their living space.
A Tyson Foods poultry plant in Springdale, Ark., had 481 infections, and 95 percent were asymptomatic.
Prisons in Arkansas, North Carolina, Ohio and Virginia counted 3,277 infected people, but 96 percent were asymptomatic.
During its seven-month global rampage, the coronavirus has claimed more than 700,000 lives. But Gandhi began to think the bigger mystery might be why it has left so many more practically unscathed.
What was it about these asymptomatic people, who lived or worked so closely to others who fell severely ill, she wondered, that protected them? Did the “dose” of their viral exposure make a difference? Was it genetics? Or might some people already have partial resistance to the virus, contrary to our initial understanding?
Efforts to understand the diversity in the illness are finally beginning to yield results, raising hope the knowledge will help accelerate development of vaccines and therapies — or possibly even create new pathways toward herd immunity in which enough of the population develops a mild version of the virus that they block further spread and the pandemic ends.
“A high rate of asymptomatic infection is a good thing,” said Gandhi, an infectious-disease specialist at the University of California at San Francisco. “It’s a good thing for the individual and a good thing for society.”
The coronavirus has left numerous clues — the uneven transmission in different parts of the world, the mostly mild impact on children. Perhaps most tantalizing is the unusually large proportion of infected people with no symptoms. The Centers for Disease Control and Prevention last month estimated that rate at about 40 percent.
Those clues have sent scientists off in different directions: Some are looking into the role of the receptor cells, which the virus uses to infiltrate the body, to better understand the role that age and genetics might play. Others are delving into face masks and whether they may filter just enough of the virus so that those wearing them had mild cases or no symptoms at all.
The theory that has generated the most excitement in recent weeks is that some people walking among us might already have partial immunity.
https://web.whatsapp.com/send?text=http://a.msn.com/05/en-us/BB17JpdS?ocid=sw
When SARS-CoV-2 was first identified on Dec. 31, 2019, public health officials deemed it a “novel” virus because it was the first time it had been seen in humans who presumably had no immunity from it whatsoever. There’s now some very early, tentative evidence suggesting that assumption might have been wrong.
One mind-blowing hypothesis — bolstered by a flurry of recent studies — is that a segment of the world’s population may have partial protection thanks to “memory” T cells, the part of our immune system trained to recognize specific invaders. This could originate from cross protection derived from standard childhood vaccinations. Or, as a paper published Tuesday in Science suggested, it could trace back to previous encounters with other coronaviruses, such as those that cause the common cold.
“This might potentially explain why some people seem to fend off the virus and may be less susceptible to becoming severely ill,” National Institutes of Health Director Francis Collins remarked in a blog post this past week.
On a population level, such findings, if validated, could be far-reaching.
Hans-Gustaf Ljunggren, a researcher at Sweden’s Karolinska Institute, and others have suggested that public immunity to the coronavirus could be significantly higher than what has been suggested by serology studies. In communities in Boston, Barcelona, Wuhan and other major cities, the proportion of people estimated to have antibodies and therefore presumably be immune has mostly been in the single digits. But if others had partial protection from T cells, that would raise a community’s immunity level much higher.
This, Ljunggren said, would be “very good news from a public health perspective.”
Some experts have gone so far as to speculate whether some surprising recent trends in the epidemiology of the coronavirus — the drop in infection rates in Sweden where there have been no widespread lockdowns or mask requirements, or the high rates of infection in Mumbai’s poor areas but little serious disease — might be due to preexisting immunity.
Others say it’s far too early to draw such conclusions. Anthony S. Fauci, the United States’ top infectious-disease expert, said in an interview that while these ideas are being intensely studied, such theories are premature. He agreed that at least some partial preexisting immunity in some individuals seems a possibility.
And he said the amount of virus someone is exposed to — called the inoculum — “is almost certainly an important and likely factor” based on what we know about other viruses.
But Fauci cautioned there are multiple likely reasons — including youth and general health — that determine whether a particular individual shrugs off the disease or dies of it. He also emphasized that even those with mild illness may have lingering medical issues.
That reinforces the need, in his view, for continued vigilance in social distancing, masking and other precautions.
“There are so many other unknown factors that maybe determine why someone gets an asymptomatic infection,” Fauci said. “It’s a very difficult problem to pinpoint one thing.”
Immune memory machine
News headlines have touted the idea based on blood tests that 20 percent of some New York communities might be immune, 7.3 percent in Stockholm, 7.1 percent in Barcelona. Those numbers come from looking at antibodies in people’s blood that typically develop after they are exposed to a virus. But scientists believe another part of our immune system — T cells, a type of white blood cell that orchestrates the entire immune system — could be even more important in fighting against the coronavirus.
Recent studies have suggested that antibodies from the coronavirus seem to stick around for only two to three months in some people. While work on T cells and the coronavirus is only getting started — testing T cells is much more laborious than antibody testing — previous research has shown that, in general, T cells tend to last years longer.
One of the first peer-reviewed studies on the coronavirus and T cells was published in mid-May in the journal Cell by Alessandro Sette, Shane Crotty and others at the La Jolla Institute for Immunology near San Diego.
The group was researching blood from people who were recovering from coronavirus infections and wanted to compare that to samples from uninfected controls who were donors to a blood bank from 2015 to 2018. The researchers were floored to find that in 40 to 60 percent of the old samples, the T cells seemed to recognize SARS-CoV-2.
“The virus didn’t even exist back then, so to have this immune response was remarkable,” Sette said.
Research teams from five other locations reported similar findings. In a study from the Netherlands, T cells reacted to the virus in 20 percent of the samples. In Germany, 34 percent. In Singapore, 50 percent.
The different teams hypothesized this could be due to previous exposure to similar pathogens. Perhaps fortuitously, SARS-CoV-2 is part of a large family of viruses. Two of them — SARS and MERS — are deadly and led to relatively brief and contained outbreaks. Four other coronavirus variants, which cause the common cold, circulate widely each year but typically result in only mild symptoms. Sette calls them the “less-evil cousins of SARS-CoV-2.”
This week, Sette and others from the team reported new research in Science providing evidence the T cell responses may derive in part from memory of “common cold” coronaviruses.
“The immune system is basically a memory machine,” he said. “It remembers and fights back stronger.”
Interestingly, the researchers noted in their paper, the strongest reaction they saw was against the spike proteins that the virus uses to gain access to cells — suggesting that fewer viral copies get past these defenses.
“The current model assumes you are either protected or you are not — that it’s a yes or no thing,” Sette added. “But if some people have some level of preexisting immunity, that may suggest it’s not a switch but more continuous.”
Childhood vaccines

Nearly 2,000 miles away, at the Mayo Clinic in Rochester, Minn., Andrew Badley was zeroing in the possible protective effects of vaccines.
Teaming up with data experts from nference, a company that manages their clinical data, he and other scientists looked at records from 137,037 patients treated at the health system to look for relationships between vaccinations and coronavirus infection.
They knew that the vaccine for smallpox, for example, had been shown to protect against measles and whooping cough. Today, a number of existing vaccines are being studied to see if any might offer cross-protection against SARS-CoV-2.
The results were intriguing: Seven types of vaccines given one, two or five years in the past were associated with having a lower rate of infection with the new coronavirus. Two vaccines in particular seemed to show stronger links: People who got a pneumonia vaccine in the recent past appeared to have a 28 percent reduction in coronavirus risk. Those who got polio vaccines had a 43 percent reduction in risk.
Venky Soundararajan, chief scientific officer of nference, remembers when he first saw how large the reduction appeared to be, he immediately picked up his phone and called Badley: “I said, ‘Is this even possible?’”
The team looked at dozens of other possible explanations for the difference. They adjusted for geographic incidence of the coronavirus, demographics, comorbidities, even whether people had had mammograms or colonoscopies under the assumption that people who got preventive care might be more apt to social distance. But the risk reduction still remained large.
“This surprised us completely,” Soundararajan recalled. “Going in we didn’t expect anything or maybe one or two vaccines showing modest levels of protection.”
The study is only observational and cannot show a causal link by design, but Mayo researchers are looking at a way to quantify the activity of these vaccines on the coronavirus to serve as a benchmark to the new vaccines being created by companies such as Moderna. If existing vaccines appear as protective as new ones under development, he said, they could change the world’s whole vaccine strategy.
Genetics and biology
Click to expand
The novel coronavirus is a master of disguise: Here's how it works
At NIH headquarters in Bethesda, Md., meanwhile, Alkis Togias has been laser-focused on one group of the mildly impacted: children. He wondered if it might have something to do with the receptor known as ACE2, through which the virus hitchhikes into the body.
In healthy people, the ACE2 receptors perform the important function of keeping blood pressure stable. The novel coronavirus latches itself to ACE2, where it replicates. Pharmaceutical companies are trying to figure out how to minimize the receptors or to trick the virus into attaching itself to a drug so it doesn’t replicate and travel throughout the body.
Was it possible, Togias asked, that children naturally expressed the receptor in a way that makes them less vulnerable to infection?
He said recent papers have produced counterintuitive findings about one subgroup of children — those with a lot of allergies and asthma. The ACE2 receptors in those children were diminished, and when they were exposed to an allergen such as cat hair, the receptors were further reduced. Those findings, combined with data from hospitals showing that asthma did not seem to be a risk factor for the respiratory virus, as expected, have intrigued researchers.
“We are thinking allergic reactions may protect you by down-regulating the receptor,” he said. “It’s only a theory of course.”
Togias, who is in charge of airway biology for the National Institute of Allergy and Infectious Diseases, is looking at how those receptors seem to be expressed differently as people age, as part of a study of 2,000 U.S. families. By comparing those differences and immune responses within families, they hope to be able to better understand the receptors’ role.
Separately, a number of genetic studies show variations in genes associated with ACE2 with people from certain geographic areas, such as Italy and parts of Asia, having distinct mutations. No one knows what significance, if any, these differences have on infection, but it’s an active area of discussion in the scientific community.
Masks

Before the pandemic, Gandhi, the University of California researcher, specialized in HIV. But like other infectious-disease experts these days, she has spent many of her waking hours thinking about the coronavirus. And in scrutinizing the data on outbreaks one day, she noticed what might be a pattern: People were wearing masks in the settings with the highest percentage of asymptomatic cases.
The numbers on two cruise ships were especially striking. In the Diamond Princess, where masks weren’t used and the virus was likely to have roamed free, 47 percent of those tested were asymptomatic. But in the Antarctic-bound Argentine cruise ship, where an outbreak hit in mid-March and surgical masks were given to all passengers and N95 masks to the crew, 81 percent were asymptomatic.
Similarly high rates of asymptomatic infection were documented at a pediatric dialysis unit in Indiana, a seafood plant in Oregon and a hair salon in Missouri, all of which used masks. Gandhi was also intrigued by countries such as Singapore, Vietnam and the Czech Republic that had population-level masking.
“They got cases,” she noted, “but fewer deaths.”
The scientific literature on viral dose goes back to around 1938 when scientists began to find evidence that being exposed to one copy of a virus is more easily overcome than being exposed to a billion copies. Researchers refer to the infectious dose as ID50 — or the dose at which 50 percent of the population would become infected.
While we don’t know what that level might be for the coronavirus (it would be unethical to expose humans in this way), previous work on other nonlethal viruses showed that people tend to get less sick with lower doses and more sick with higher doses. A study published in late May involving hamsters, masks and SARS-CoV-2 found those given coverings had milder cases than those who did not get them.
In an article published this month in the Journal of General Internal Medicine, Gandhi noted that in some outbreaks early in the pandemic in which most people did not wear masks, 15 percent of the infected were asymptomatic. But later on, when people began wearing masks, the rate of asymptomatic people was 40 to 45 percent.
She said the evidence points to masks not just protecting others — as U.S. health officials emphasize — but protecting the wearer as well. Gandhi makes the controversial argument that while we’ve mostly talked about asymptomatic infections as terrifying due to how people can spread the virus unwittingly, it could end up being a good thing.
“It is an intriguing hypothesis that asymptomatic infection triggering immunity may lead us to get more population-level immunity,” Gandhi said. “That itself will limit spread.”
coronavirus-infections-have-no-symptoms-might-they-be-the-key-to-ending-the-pandemic/ar-BB17JpdS?ocid=sf
Attachments
‘A Smoking Gun’: Infectious Coronavirus Retrieved From Hospital Air
Airborne virus plays a significant role in community transmission, many experts believe. A new study fills in the missing piece: Floating virus can infect cells.
Image
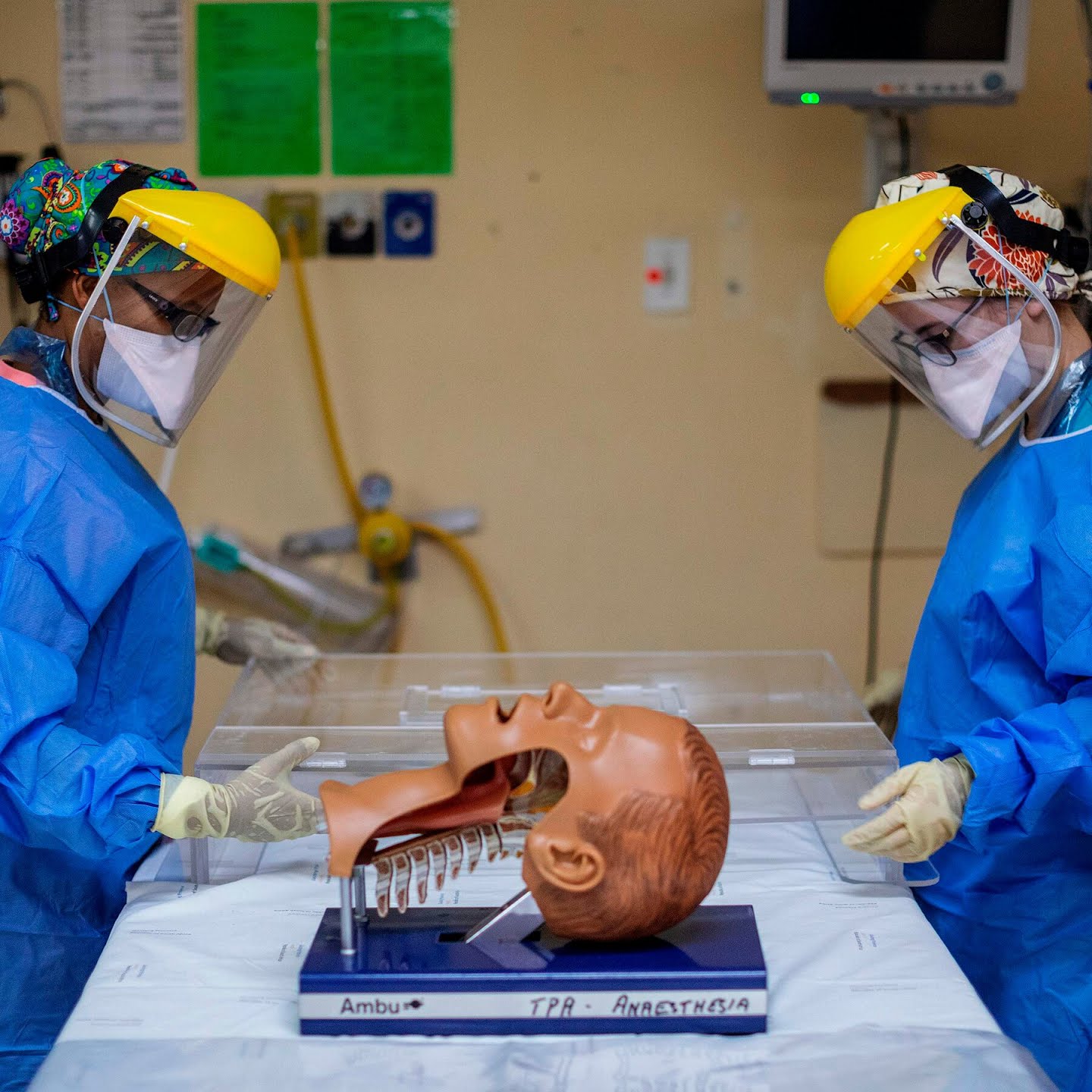
Doctors in Johannesburg demonstrated how to place a device called an intubox over a patient, to help curb the spread of viral droplets during intubation.Credit...Michele Spatari/Agence France-Presse — Getty Images
By Apoorva Mandavilli
Aug. 11, 2020
Skeptics of the notion that the coronavirus spreads through the air — including many expert advisers to the World Health Organization — have held out for one missing piece of evidence: proof that floating respiratory droplets called aerosols contain live virus, and not just fragments of genetic material.
Now a team of virologists and aerosol scientists has produced exactly that: confirmation of infectious virus in the air.
“This is what people have been clamoring for,” said Linsey Marr, an expert in airborne spread of viruses who was not involved in the work. “It’s unambiguous evidence that there is infectious virus in aerosols.”
A research team at the University of Florida succeeded in isolating live virus from aerosols collected at a distance of seven to 16 feet from patients hospitalized with Covid-19 — farther than the six feet recommended in social distancing guidelines.
The findings, posted online last week, have not yet been vetted by peer review, but have already caused something of a stir among scientists. “If this isn’t a smoking gun, then I don’t know what is,” Dr. Marr tweeted last week.
But some experts said it still was not clear that the amount of virus recovered was sufficient to cause infection.
The research was exacting. Aerosols are minute by definition, measuring only up to five micrometers across; evaporation can make them even smaller. Attempts to capture these delicate droplets usually damage the virus they contain.
“It’s very hard to sample biological material from the air and have it be viable,” said Shelly Miller, an environmental engineer at the University of Colorado Boulder who studies air quality and airborne diseases.
 www.google.com
www.google.com
Airborne virus plays a significant role in community transmission, many experts believe. A new study fills in the missing piece: Floating virus can infect cells.
Image

Doctors in Johannesburg demonstrated how to place a device called an intubox over a patient, to help curb the spread of viral droplets during intubation.Credit...Michele Spatari/Agence France-Presse — Getty Images
By Apoorva Mandavilli
Aug. 11, 2020
Skeptics of the notion that the coronavirus spreads through the air — including many expert advisers to the World Health Organization — have held out for one missing piece of evidence: proof that floating respiratory droplets called aerosols contain live virus, and not just fragments of genetic material.
Now a team of virologists and aerosol scientists has produced exactly that: confirmation of infectious virus in the air.
“This is what people have been clamoring for,” said Linsey Marr, an expert in airborne spread of viruses who was not involved in the work. “It’s unambiguous evidence that there is infectious virus in aerosols.”
A research team at the University of Florida succeeded in isolating live virus from aerosols collected at a distance of seven to 16 feet from patients hospitalized with Covid-19 — farther than the six feet recommended in social distancing guidelines.
The findings, posted online last week, have not yet been vetted by peer review, but have already caused something of a stir among scientists. “If this isn’t a smoking gun, then I don’t know what is,” Dr. Marr tweeted last week.
But some experts said it still was not clear that the amount of virus recovered was sufficient to cause infection.
The research was exacting. Aerosols are minute by definition, measuring only up to five micrometers across; evaporation can make them even smaller. Attempts to capture these delicate droplets usually damage the virus they contain.
“It’s very hard to sample biological material from the air and have it be viable,” said Shelly Miller, an environmental engineer at the University of Colorado Boulder who studies air quality and airborne diseases.

‘A Smoking Gun’: Infectious Coronavirus Retrieved From Hospital Air (Published 2020)
Airborne virus plays a significant role in community transmission, many experts believe. A new study fills in the missing piece: Floating virus can infect cells.
FDA authorizes potentially pandemic-changing saliva test
The Food and Drug Administration on Saturday issued an emergency use authorization for the SalivaDirect COVID-19 diagnostic test developed by the Yale School of Public Health in partnership with the National Basketball Association.
The test processes saliva to rapidly determine whether a person has been infected with the coronavirus and does not require any type of swab or specific collection device. Andy Slavitt, a former acting administrator for the Centers for Medicare and Medicaid Services under the Obama administration, said the test has a chance to become one of the first "major game changers in fighting the pandemic."
He praised the physical comfort level of the test, as well its affordability, turnaround time, and accuracy, noting that it could come in handy for schools, universities, and office buildings.
Source: The Week, Food and Drug Administration
The Food and Drug Administration on Saturday issued an emergency use authorization for the SalivaDirect COVID-19 diagnostic test developed by the Yale School of Public Health in partnership with the National Basketball Association.
The test processes saliva to rapidly determine whether a person has been infected with the coronavirus and does not require any type of swab or specific collection device. Andy Slavitt, a former acting administrator for the Centers for Medicare and Medicaid Services under the Obama administration, said the test has a chance to become one of the first "major game changers in fighting the pandemic."
He praised the physical comfort level of the test, as well its affordability, turnaround time, and accuracy, noting that it could come in handy for schools, universities, and office buildings.
Source: The Week, Food and Drug Administration
Yale's COVID-19 saliva test used in NBA gets FDA emergency approval
University researchers who developed the test said they don't intend to commercialize it.
Federal officials have given emergency approval to a coronavirus saliva test that Yale University researchers used on NBA players and staff.
In a statement, Stephen Hahn, commissioner of the Food and Drug Administration, called the test "groundbreaking," partly because it doesn't need additional components, which have been prone to shortages, necessary with the standard nasal swab COVID-19 test.
The test, known as SalivaDirect, "is simpler, less expensive, and less invasive than the traditional method for such testing," Yale said in a news release Saturday.
The authorization allows the test to bypass the FDA's regular approval process.
Full coverage of the coronavirus outbreak
SalivaDirect doesn't rely on proprietary technology, and Yale researchers don't intend to commercialize it, the university said. The researchers will provide protocols to other diagnostic laboratories that could use commercially available equipment to conduct the test, the agency said.
Nathan Grubaugh, one of the researchers who developed the test, said he expects labs to charge about $10 per sample.
"If cheap alternatives like SalivaDirect can be implemented across the country, we may finally get a handle on this pandemic, even before a vaccine," Grubaugh said, according to the Yale news release.
Yale announced the study in June. The researchers partnered with the NBA because its players and on-court staff members are tested regularly, they're in close contact with one another, and they don't wear face coverings.
Yale said the accuracy of the results, which haven't yet been peer-reviewed, was similar to that of nasal swab tests.

 www.nbcnews.com
www.nbcnews.com
University researchers who developed the test said they don't intend to commercialize it.
Federal officials have given emergency approval to a coronavirus saliva test that Yale University researchers used on NBA players and staff.
In a statement, Stephen Hahn, commissioner of the Food and Drug Administration, called the test "groundbreaking," partly because it doesn't need additional components, which have been prone to shortages, necessary with the standard nasal swab COVID-19 test.
The test, known as SalivaDirect, "is simpler, less expensive, and less invasive than the traditional method for such testing," Yale said in a news release Saturday.
The authorization allows the test to bypass the FDA's regular approval process.
Full coverage of the coronavirus outbreak
SalivaDirect doesn't rely on proprietary technology, and Yale researchers don't intend to commercialize it, the university said. The researchers will provide protocols to other diagnostic laboratories that could use commercially available equipment to conduct the test, the agency said.
Nathan Grubaugh, one of the researchers who developed the test, said he expects labs to charge about $10 per sample.
"If cheap alternatives like SalivaDirect can be implemented across the country, we may finally get a handle on this pandemic, even before a vaccine," Grubaugh said, according to the Yale news release.
Yale announced the study in June. The researchers partnered with the NBA because its players and on-court staff members are tested regularly, they're in close contact with one another, and they don't wear face coverings.
Yale said the accuracy of the results, which haven't yet been peer-reviewed, was similar to that of nasal swab tests.

FDA approves emergency use of Yale's COVID-19 saliva test used in NBA
University researchers who developed the test said they don't intend to commercialize it.
















