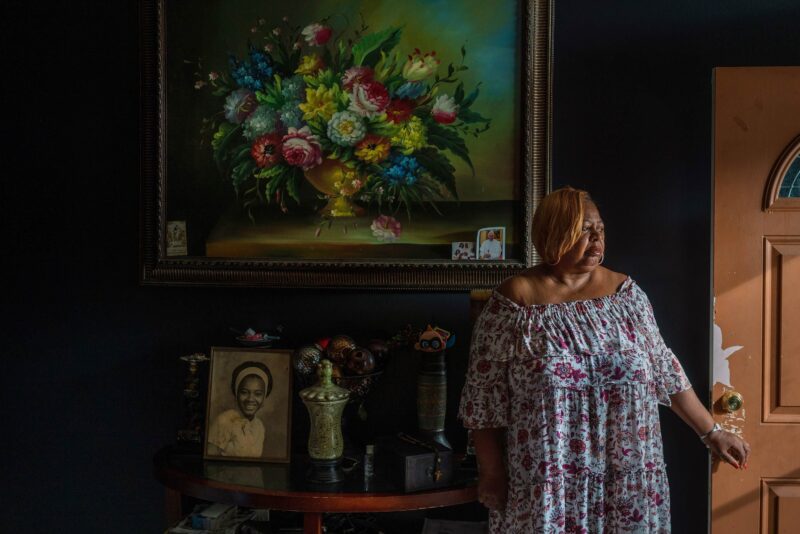Sent Home to Die
In New Orleans, hospitals sent patients infected with the coronavirus into hospice facilities or back to their families to die at home, in some cases discontinuing treatment even as relatives begged them to keep trying.
Rodney Lavalais holds a photo of his mother, Sarah Johnson, outside her New Orleans home
In New Orleans, hospitals sent patients infected with the coronavirus into hospice facilities or back to their families to die at home, in some cases discontinuing treatment even as relatives begged them to keep trying.

www.propublica.org
Sarah Johnson spent her entire life taking care of people — the six children she raised, mostly alone, and the hospital patients she served in her 25 years as a nurse. But at 86, she was the one who needed care. She was thin and frail and had COVID-19.
Her son Rodney Lavalais anguished over the fact that she was all by herself; he’d moved in with her four years ago after he saw her struggling to open a jar. But when the ambulance took her to Ochsner West Bank, a hospital in the New Orleans suburbs, he couldn’t come with her.
He couldn’t see how stretched the hospital was in mid-April, as the coronavirus surged through the city and flooded its intensive care unit to capacity. Nor could he speak up for his mother when a doctor asked her questions she couldn’t answer.
When he and his siblings received a call from the hospital only 23 hours after she was admitted, informing them there was nothing more doctors could do, they were devastated. Their mother was breathing on her own, but her kidneys were failing. “They told us we couldn’t see her, and that maybe contributed to our decision to bring her home,” he said. “They said hospice will be there to make sure she’s comfortable.”
In that moment, Ochsner made a decision in stark contrast to those made by other hospitals in COVID-19 hot spots across the country: At a time when relatives were being kept away from their sick loved ones to prevent the spread of a contagious and deadly virus, Ochsner sent infected patients back into communities to die at home, and be cared for by untrained family members without the proper protective equipment.
Under normal conditions, hospice workers make frequent face-to-face visits, especially in a patient’s final days. But during the pandemic, when hospice companies were limiting in-person visits, Johnson’s family was left to spend her last days alone with her, watching her moan, convinced she was in pain.
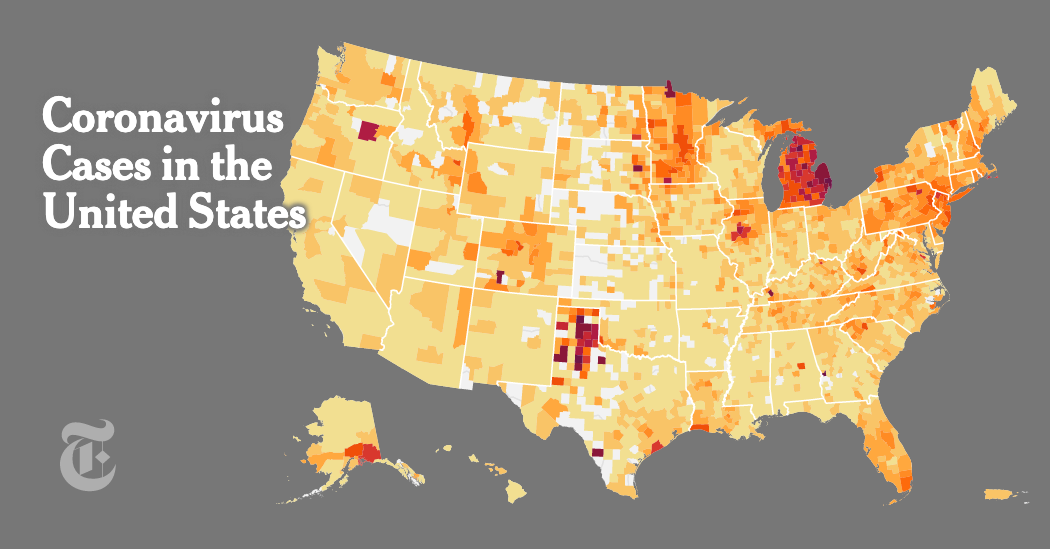
The city’s death statistics reveal an aberration, ProPublica found. Nationally, coronavirus patients aged 85 and older died at home only 4% of the time, according to data from the Centers for Disease Control and Prevention; local coroner records show that in New Orleans, it was 17%. Reporters attempted to contact the families of everyone who died at home there.
The interviews revealed a striking pattern: Before they died, about two dozen patients first sought care at a hospital, which then discharged them, in many cases sending them home to die with hospice care. All were Black. The vast majority came from Ochsner Health, the largest hospital network in Louisiana, which treated 60% of the region’s critically ill coronavirus patients.
The families of eight patients, as young as 69, told ProPublica that Ochsner staff pressured them into accepting hospice care for their loved ones who had COVID-19, even as some questioned or pushed back against the suggestion. Three families said they were told that there wasn’t enough space to continue treating the patient in the hospital, or that the hospital needed the bed for another patient.
Some family members felt that their loved ones suffered without hospice workers at their side to manage their pain and navigate their complex symptoms. At least two relatives got sick, after being denied the proper protective gear.
It hurt enough for Johnson’s children to lose her, but then, there was what her medical records revealed: That the decision to recommend hospice was influenced by a doctor’s questionable speculation on her mental capacity; that on the day she was discharged home, her kidneys had improved to the point that she was no longer in renal failure; that with additional treatment, according to one expert who reviewed her case for ProPublica, she probably could have survived.
Even though Johnson’s son signed a waiver permitting Ochsner to discuss her treatment with ProPublica, officials did not respond to questions about her care, stating they do “not believe that, ethically or legally, a waiver by a family member of these protections on behalf of a deceased patient equate to our ability to speak freely to the general public about the patient’s care.”
Ochsner did not answer ProPublica’s questions about families feeling pressured into hospice. These are always difficult discussions, a spokesperson said, and with the rapid deterioration of COVID-19 patients, relatives often had to make end-of-life decisions more quickly than with other illnesses. In an email, the spokesperson said the pandemic’s strains on staffing and supply levels had no influence on care: “We do not and did not cut corners on our patient’s care at any time during or after COVID-19.”
Prior to the pandemic, an increasing number of people were choosing to die at home, bolstered by a growing hospice movement. But data reveals that during the pandemic, the trend has flipped, with most COVID-19 deaths occurring in the hospital due to the “acuity of the illness, the rapid decline and the severity of illness,” said Dr. Sadiya Khan, an assistant professor of cardiology and preventive medicine at Northwestern University’s Feinberg School of Medicine, whose recent
research has analyzed the locations of COVID deaths. In areas where many home deaths occurred, Khan said that it’s “a signal that there was potentially an overwhelmed health care system.”
Hospitals in Seattle, Chicago and New York City, three other early hotspots, told ProPublica they did not send patients home for hospice care, in part because of the threat of infection to vulnerable caretakers, and in part because of the harrowing deaths that families might have to navigate mostly alone.
“You have to be very aggressive in terms of getting ahead of symptoms, because with COVID, once that shortness of breath starts, it’s very hard to control,” said Dr. Darrell Owens, a doctor of nursing practice who runs palliative and supportive care at the University of Washington Medical Center-Northwest in Seattle. He said he would be “very worried about trying to manage that” in home hospice, and that dying patients at his hospital were provided palliative support through an inpatient program.
“We sent nobody — zero — home on hospice to die of COVID.”
In mid-March, two weeks after more than a million people descended on New Orleans for Mardi Gras, the virus spread uncontrollably and exponentially across the city, marking it as an early hotspot for COVID-19.
Lavalais moved in with his mother four years ago after he saw her struggling to open a jar.
Sarah Johnson knew what that meant for someone her age. Her phone conversations with friends, about the intrigues of “The Young and the Restless,” started to drift toward the new threat. “We talked about it and how we had to be careful,” said her cousin Lois Smith. “I was a little more conscious about visitors, but she still had them.”
Grandchildren stopped by; two of her sons saw her almost daily. Johnson’s daughter would drive her around town, letting her tour her old neighborhoods from the safety of the car.
Despite the physical limitations that came with aging — she could no longer bear to sit in church pews with her bad back — she remained the independent woman who had put herself through nursing school and bought a home with cash, so adamant about avoiding debt that she sometimes paid bills up to a year in advance. She still balanced her checkbook, and spent her days doing crossword puzzles and poring over her Bible.
So when she grew too weak to get out of bed, her children knew something was wrong. After several days, her family called an ambulance. Emergency medical technicians concluded her blood oxygen saturation was low enough that she required hospital care. On the afternoon of April 16, they dropped her off at Ochsner West Bank.
The hospital was slammed. To accommodate the influx of patients, Ochsner was converting operating rooms into makeshift intensive care units. But even so, earlier that week, Ochsner West Bank’s ICU reached 100% capacity, according to
state data obtained by the Documenting COVID-19 project at the Brown Institute for Media Innovation. Nurses at West Bank told ProPublica that there was a period during the surge when every ventilator was in use, with critically ill patients waiting in line.
One nurse said that her middle-aged patient died while waiting for a ventilator. “That was the hardest one,” the nurse told ProPublica. “I fought to get them a vent all day.”
Ochsner denies this. “We did not triage or ration the utilization of ventilators,” a spokesperson said. “All patients who required ventilation received that care in a timely fashion.”
As capacity shrunk, Ochsner employees adopted an unusual method to withhold life-sustaining care from patients with poor prognoses, several told ProPublica. In some cases, doctors gave patients do-not-resuscitate orders without family or patient consent, sometimes overruling families that wanted everything done for their loved one, three nurses said.
In 2016, a top Ochsner attorney published an
article in Ochsner’s
medical journal that asked what doctors should do when they believe “any clinical treatment other than comfort care will be ineffective or harmful to a patient” but the patient’s family is “in support of ‘doing everything.’” The lawyer wrote that it would be “prudent” to have two doctors sign off before implementing a do-not-resuscitate order unilaterally.
During the pandemic, three nurses across the hospital system told ProPublica they’d seen cases where two doctors signed off to give COVID-19 patients a do-not-resuscitate status without the patient or family’s agreement. For the sickest ones, they said, this effectively meant the hospital was withdrawing care, since a patient sick enough to need a ventilator was unlikely to survive without one and they generally wouldn’t intubate someone with a DNR.
“You get the family that says absolutely not — we want you to do everything,” one nurse at Ochsner West Bank told ProPublica. “When there’s enough vents,” the nurse said, doctors will respect the family’s wishes even if they disagree with them. “But when your decision is impacting other people, we can’t keep doing care.”
Ochsner denies that its employees issued any do-not-resuscitate orders unilaterally. “DNRs are not issued without the consent of or over the objection of a patient or legally authorized representative,” an Ochsner spokesperson said. “Given these challenging and unusual times, it comes as no surprise that a member of the care team, including nursing, had a different perception of those end of life conversations, especially where they were not involved in all of the discussions and interactions.”
The last time New Orleans health care workers faced a crisis like this was Hurricane Katrina, when floodwaters
knocked out the power at several hospitals, leaving patients and staff marooned. At Memorial Hospital, which was owned by a different company at the time, several DNR patients died after doctors
injected them with high doses of morphine. In the aftermath, Memorial’s parent company sold Memorial and two other hospitals, including what is now known as West Bank, to Ochsner, which began a period of
expansion in which it would become the largest hospital network in the state.
During the spring surge of the virus,
staffing was among the Ochsner system’s most pressing concerns. As early as March 25, about
60 Ochsner employees had tested positive and hundreds more were out on quarantine. The system repurposed staff from its closed outpatient clinics, and recruited an additional 140 nurses from other locations. “We adapted our staffing plans as needed to avoid little to no disruption to the quality of patient care,” the spokesperson said.
ProPublica spoke with more than two dozen doctors, nurses, and other healthcare workers at Ochsner about their experiences during the pandemic. All asked that their names be withheld, to not jeopardize their employment. Many described how limited time and resources prevented them from giving the level of care they were accustomed to, and in some cases forced them to ration treatment.
“If I could’ve doubled myself, I could’ve saved some people,” a nurse at Ochsner Baptist told ProPublica. With critically ill dialysis patients, the nurse would normally carefully monitor their machines, tweaking their levels before anything could cause a problem. “But I can’t be everywhere. My other patient is coding. So I’m just going from code to code to code.”
Despite the chaos, Johnson was evaluated within minutes, tested for the virus and hooked up to intravenous fluids. Dr. Charlane Liles noted that she was “markedly dehydrated” and her heart rhythm was fast and irregular — a problem likely caused by the virus, an Ochsner cardiologist later determined. She was alert and oriented, though, and her breathing was normal. And thanks to a breathing tube in her nose, the mildest option for treating lung problems, her oxygen levels had improved to almost 100%.
But her labs revealed another problem: Johnson — who already had modest chronic kidney disease — was now in acute renal failure, a common consequence of COVID-19, which can severely damage kidneys. Doctors agreed that they needed to treat Johnson’s dehydration. Liles admitted Johnson to the hospital so she could continue getting oxygen, fluids and heart medication and receive “close monitoring.”
Overnight, a nurse turned off her oxygen, letting her breathe on her own, because Johnson no longer needed the help.
As the sun rose, a new series of medical experts began to evaluate her.
First was Zannah Richard, a dietitian, who had been asked to determine if Johnson was malnourished; at 106 pounds, she was thin, and her labs revealed depleted levels of albumin, a liver protein for which low levels can be a sign of malnutrition but is also associated with
kidney disease and other illnesses.
While Johnson could be at risk of being underweight, Richard determined, she was not malnourished. The dietitian left her recommendations for Johnson on sticky notes and filed them electronically.
Three hours later, without physically examining Johnson, citing coronavirus protocols, nephrologist Dr. Miguel Molina reviewed her records and determined she was not a dialysis candidate. Experts told ProPublica this was likely because she was not sick enough for dialysis. Molina then decided to take her off of fluids.
Shortly thereafter, around 10:30 a.m., Dr. Amanda Cruz-Cruz entered Johnson’s room for a more general evaluation. Johnson was asleep when she came in, but the physician awoke her easily. Johnson asked for some water, and while she appeared attentive, her speech was delayed, her memory impaired and she was unable to “hold a meaningful conversation,” the doctor noted. When another doctor had tried to take her medical history the night before, Johnson was too confused to provide it.
Cruz-Cruz then proceeded to make a series of judgments that several experts told ProPublica confused them and, in some instances, appeared inappropriate.
“Based on physical appearance and presentation, patient likely has advanced [or] end stage dementia,” Cruz-Cruz wrote, suggesting that her dementia was likely so bad that even before she contracted the coronavirus, she had been bed bound and incapacitated. At this point, according to the medical notes, no one at the hospital had spoken to her children about her mental state.
ProPublica interviewed seven relatives and friends who saw or spoke with her regularly; while she sometimes misplaced keys or repeated childhood stories — indicating to her family that she might be in the early stages of dementia — they all said she was still sharp, and not at all incapacitated until she contracted COVID-19.
The assessment also went against what seven geriatricians described as well-established best practices in geriatric medicine. “You shouldn’t be diagnosing dementia in the acute setting,” said Dr. Louise Aronson, a professor of medicine at the University of California, San Francisco Division of Geriatrics and author of “Elderhood,” a finalist for the Pulitzer Prize. The prevalence of delirium is
high with acutely ill elderly patients,
particularly those with COVID-19, and Aronson said that dementia should not be diagnosed in a “hospital setting because it’s delirium until proven otherwise.”
Cruz-Cruz also noted that Johnson was “severely malnourished.” The doctor did not explain her reasoning, and it is unclear if she was aware that the dietitian asked to evaluate Johnson for malnutrition had determined the opposite just hours earlier.
Cruz-Cruz concluded: Since she “is not candidate for dialysis if needed, is severely malnourished, [is of] advanced age, appears to have advanced dementia and functional status [is] currently poor,” Johnson would benefit from a do-not-resuscitate order and potentially should receive hospice care going forward. Cruz-Cruz did not respond to ProPublica’s questions.
Shortly thereafter, a nurse noted that palliative care specialists had been consulted to determine if Johnson’s family would consent to a DNR, “which in turn will determine plan of care.”
At 2 p.m., Crystal Burke, a nurse practitioner specialized in palliative care, called Lavalais and his siblings. According to her notes, she told the family Johnson’s prognosis was “poor” and they discussed what would be best for her in light of her “dementia, renal failure, respiratory failure, and malnutrition.” Burke explained how hospice can “help [a] patient live with the best quality of life possible,” and the family agreed to go along with the plan.
Rodney Lavalais couldn’t join his mother at the hospital.
Lavalais does not remember anyone mentioning advanced dementia or malnutrition, and was surprised by Burke’s record of the conversation. Burke did not respond to ProPublica’s questions about Johnson’s care. According to the family, they were told that their mother had COVID-19, her kidneys were failing and she was going to die, and that there was nothing the hospital could do to save her.
With the children’s approval, at 4:18 p.m., a social worker faxed a referral to Compassus, a national, for-profit company that provides hospice care and has an office in the New Orleans suburbs. It was late on a Friday afternoon, and Johnson stayed at the hospital over the weekend.
By Monday morning, a new set of labs returned. Two experts who reviewed Johnson’s medical records for ProPublica said that the tests showed her kidney function had improved remarkably, not close to normal levels but enough so that she was no longer in kidney failure. Additionally, her electrocardiogram showed that her heartbeat had gone back to normal, beating healthily throughout the day. But a new problem had arisen: her sodium levels were rising precipitously. Generally caused by dehydration,
high sodium can make people confused and erratic, and if
untreated, can result in coma or death.
None of the doctors at Ochsner noted that Johnson’s chief medical problems were improving, or her concerning sodium increase, in more than 650 pages of detailed medical records from her stay. In a discharge summary hours later, Dr. Diane Van Gerwen, who did not respond to ProPublica’s questions, even wrote that Johnson’s heartbeat was still fast and irregular and that her “renal failure [was] not improving but not worsening.”
Then, as
required under Medicare, Van Gerwen documented the reasons Johnson needed hospice care, citing her kidney problems as the main reason, along with dementia and a general “failure to thrive.” At 6 p.m., Johnson was discharged.
“If she stayed in a few more days and got more IV fluid, I think she would’ve done fine,” said Dr. Brobson Lutz, an infectious disease doctor on staff at Ochsner, who served as the New Orleans Director of Health for 13 years and reviewed the case for ProPublica. “She was only mildly symptomatic for COVID. She was certainly getting better and responding.”
Lutz thinks the decision to move to hospice rather than monitor her probably worsened Johnson’s chances significantly. “She didn’t meet hospice criteria, renal failure not needing dialysis,” he said. “When she went home, she probably got more dehydrated. That sodium of 150 was pretty high.”
Dr. David Goldfarb, clinical director of the nephrology division at NYU Langone Health in New York City, said her kidney injury wasn’t severe enough to necessitate hospice. “She has pretty bad kidney function, but she’s not going to die of kidney failure,” he told ProPublica. “The acute kidney injury wasn’t bad enough to really make sense as a hospice diagnosis.”
In keeping with national criteria, Ochsner’s spokesperson said, “hospice was determined and recommended by the care team if the patient had a life-limiting illness in which death is anticipated in the next six months.”
As an 86-year old with COVID-19 and kidney problems, Johnson’s long-term life expectancy was not good, Goldfarb said. “Would you be surprised if this patient died in six months? Probably most doctors would say no,” he told ProPublica. “On the other hand, could she live for another year? I wouldn’t be surprised by that, either.”
For that reason, it was not unreasonable for Ochsner to suggest hospice, Goldfarb said. But that was not the only option, and he said the family should have had a choice.
A box holds the remains of Lionel Ferdinand, who died at home of COVID-19.
To understand why so many people died outside of hospitals in New Orleans, ProPublica analyzed local coroner records of the city’s more than 460 deaths through early May. An overwhelming majority, 384, died in a hospital; an additional 21, in nursing homes or an assisted living facility.
ProPublica focused on those who remained — the 55 people who died outside of any acute care setting, in categories the coroner labeled “decedent residence,” “hospice” and “other care center,” which often included hospice deaths. Reporters attempted to reach every one of their families, and spoke with 35 of them.
Experiences seemed divided along racial lines.
While Black people died from the virus at a disproportionate rate in New Orleans, white people died outside of hospitals at a higher rate than Black people. In the cases ProPublica examined, this was by choice. Reporters spoke with three families of white people who died with home or hospice care; their families said they chose to avoid the hospital and made arrangements to stay home instead. Some Black patients also stayed home, and did not seek care at the hospital.
Twenty-five families told ProPublica the deaths of their loved ones occurred after the patient sought care at a hospital. All 25 patients were Black.
A few were told they were not sick enough to be admitted, and then died at home. But 18 of the 25 Black patients were sent by a hospital to die under hospice care, according to their families. The vast majority came from Ochsner facilities.
The families of eight Black patients said they felt pressured by Ochsner staff into accepting hospice care for their loved ones.
Erma Winston’s children remain convinced that Ochsner pushed their 83-year old mother into hospice because resources were limited and she had no family at her bedside to advocate for her. Her adult granddaughter Chantell, who was involved in conversations around her care, believes she could’ve gotten better treatment. “Do I think this would have happened if COVID wasn’t going on? No, because we would have been right by her side.”
In early April, her grandmother was taken in an ambulance to Ochsner’s main campus with coronavirus symptoms. When a nurse helped Winston video chat with her family about five days later, she appeared transformed. The former postal worker, who lived independently at home, now could hardly speak. But she responded to her daughter’s voice and nodded along as she prayed.
A day later, Winston’s family got a call from a member of the palliative care team, recommending she move to hospice, they said. They pushed back. The family had already consented to forgo chest compressions if Winston’s heart stopped, but they were not ready to discontinue her care.
However, the hospital was adamant, her family told ProPublica, and her children came to believe that the decision to discharge their mother had already been made. According to one of her daughters, the hospital told her that Winston needed to either transfer to a hospice facility or be discharged home within the next day.
Her family agonized over the decision. They knew nothing about the pop-up hospice unit, which a private company had set up in a matter of days to care for COVID-19 patients in vacant space at another hospital. At the same time, if their mom came home, the whole family could get sick. They begged a social worker for more time to think. But the family said their requests seemed to fall on deaf ears. “They were definitely rushed,” Chantell said. “They could have kept her there a couple more days until we made a decision.”
The next day, Winston was transferred to the hospice unit, where about 10 days later, she died.
“It was poor management,” Chantell told ProPublica. “And sometimes with poor management, African Americans suffer.”
Ochsner Health declined to comment on Winston’s care, citing privacy restrictions. A spokesperson said that Black patients had “disproportionate
rates of infection, hospitalization and deaths,” and that they seemed to be sicker when they arrived in the emergency room, with “a higher rate of kidney and liver function abnormalities.”
The spokesperson did not respond to ProPublica’s questions about racial disparities and hospice referrals, but said that “the disparities in health that we see among the Black population are something we’ve known for decades and COVID-19 has opened the door for more people to become infected, but also an opportunity to address disparities head on and initiate change.”
Research has shown that Black families have disproportionately negative experiences with end-of-life care. Dr. Michael C. Francis, a community physician on staff at Ochsner, told ProPublica he’s seen discrimination firsthand when his patients navigate these difficult decisions with medical teams.
“They assume that Black folks don’t know anything,” he said, “and that if the doctors do something they don’t agree with, they’re not going to do anything about it.”
Under normal circumstances, hospice care can be a blessing for dying patients, allowing them to transition surrounded by loved ones in the comfort of their own home. Through Medicare, if a patient is terminally ill and has a life expectancy of six months or less, they can access on-call nursing assistance, medical equipment and prescriptions, as well as continuous care in crisis moments when symptoms flare. About half of Medicare beneficiaries die
receiving hospice services.
But due to the coronavirus’s infectious and unpredictable nature, the use of home hospice for these patients has become contentious.
At the UW Medical Center—Northwest in Seattle, one of the earliest hotspots of the virus, patients dying of COVID-19 were kept in the hospital and provided palliative support through an inpatient program. SUNY Downstate Medical Center in New York City did the same, entirely avoiding home hospice for coronavirus patients, said Dr. Bonnie Arquilla, the hospital’s director of emergency preparedness. And Rush University Medical Center in Chicago likewise handled palliative cases in the hospital instead of sending coronavirus patients home for hospice, and allowed families to visit if a patient’s death was imminent.
An oxygen tank and other medical equipment used during Ferdinand’s final days at his home in New Orleans. The hospice company has not returned to retrieve it, the family said.
The public health risk of expecting relatives to care for dying loved ones at home would have been too high, said Dr. Paul Casey, Rush’s acting chief medical officer and an emergency room physician. “A young healthy patient that we saw and diagnosed with COVID, we’d be able to send home and say, ‘You need to quarantine yourself away from family members and others to make sure you’re not potentially impacting them,’” Casey said. “That’s very different than sending someone home to be cared for by the family where you know there will be contact in the effort of needing to take care of them.”
Some hospitals were able to continue to offer home hospice care to dying patients with COVID-19, but took measures to make sure families were prepared.
In New York City, hospices were limited in what they could do because “there just wasn’t enough personal protective equipment and, without enough PPE, they couldn’t go into homes,” said Dr. Diane E. Meier, the head of the Center to Advance Palliative Care at Mount Sinai. So Meier helped set up a 24/7 telemedicine practice with palliative doctors, nurses and physician assistants always on call for people who wanted to avoid hospital care and instead take their chances at home.
The palliative care service was available to patients from hospitals across New York City. But in a place where over 20,000 people died with COVID-19, Meier said, the palliative service had about 30 home care cases in the first couple of months of the surge.
End-of-life care is a distinctly subtle form of medicine, dependent on sensitive communication and trust between patients, families and medical staff. Even in normal times, communication does not always live up to that ideal.
Dr. William LaCorte, a New Orleans physician who works with nursing homes and hospitals, said he is often given a stack of documents outlining patients’ end-of-life goals and asked to sign them to make them official. “And I won’t,” he told ProPublica. “I say I want to talk to the family first, or to the patient — and half the time, they disagree with whatever plan of care they supposedly just said they wanted.”
The coronavirus has created new, immense barriers. Hospital visitor restrictions leave patients isolated from family members, who often lack vital information to help make complex decisions.
Touro Infirmary, another hospital in New Orleans, allowed family members to visit their loved ones in the hospital before making end-of-life decisions, said Melissa Pennebaker, a nurse practitioner on its palliative care team. “It became clear early on in this pandemic that families really needed to see their family members when making these difficult decisions,” Pennebaker told ProPublica.
At Ochsner facilities, by contrast, families generally had to make these decisions over the phone, several nurses and physicians told ProPublica. Ochsner allowed families to visit, but only after they’d decided on comfort care or when the patient was actively dying, they said.
An Ochsner spokesperson did not say whether families were permitted to visit to discuss hospice and other options, but said, “Ochsner, like many health systems and hospitals across the country and as required by [the Louisiana Department of Health] instituted a zero-visitor policy. This policy did have an exception for essential visitors that included limited visitors for end-of-life patients.”
Lionel Ferdinand’s family created a memorial collage after he died.
In late March, 66-year-old Army veteran Lionel Ferdinand spent roughly a week at Ochsner Medical Center’s main campus battling COVID-19, growing increasingly delirious. Eventually, he refused the dialysis treatment he needed to survive.
“He wasn’t in his right mind,” said his wife, Connie, who said she was told by the hospital that his organs were shutting down and nothing more could be done. Unlike other families, Connie asked if her husband could be discharged, hoping that he’d be more comfortable at home. The hospital arranged for hospice care.
The hospice and home health company AmeraCare provided the family with a hospital bed, oxygen tanks and medicine, but neither it nor Ochsner provided PPE, which was hard to come by at the beginning of the pandemic. Ferdinand’s family was worried about caring for him without protection, an AmeraCare nurse noted in his hospice records. She told them to “contact any and all resources to try to attain proper PPE.” Connie’s daughter-in-law and niece were able to track down cloth masks; another family member gave her gloves.
“They should have had everyone prepared,” said his daughter Kelly.
At home, Ferdinand declined swiftly, delirious and unable to sleep. “He looked like he was smothering himself,” said his daughter Tina. “His head was popping up. We didn’t know how to treat him or how to deal with this.”
They tried to soothe him, but because he appeared to be suffering, they called the hospice company in the middle of the night and begged for a nurse to come help. No one showed.
Alone, Tina and her mother tended to Ferdinand, trying not to think about the virus particles each cough sent flying. “I was afraid,” Tina said. “But I knew my daddy needed good care.”
About 5 p.m. the next day, a hospice nurse finally came. From the hallway, without entering his bedroom, she inspected Ferdinand and told the family he was getting ready to transition, Connie said. The visit lasted 20 minutes, according to hospice records.
For seven hours after the nurse left, Ferdinand’s family cared for him as he lay dying, sweating profusely, struggling to breathe and unresponsive. They tried to make him comfortable by opening the window, turning on a fan and continuing anti-anxiety medication, but his chest heaved in distress. Then, just after midnight, Ferdinand passed away. His family feels they weathered his death alone, unprepared to relieve his suffering.
Then, some of them fell ill.
Connie Norman, photographed in the New Orleans home where her husband, Ferdinand, died
“It felt like I was breathing water … like I was catching a heart attack” said Tina, who first showed symptoms of what she believes was COVID-19. She decided not to go to the hospital, instead isolating herself until she recovered. Ferdinand’s granddaughter also fell ill.
In moments like Ferdinand’s first night at home, when family caretakers struggle to control severe symptoms, face-to-face visits from hospice workers become crucial, said Dr. Joan Teno, a medical professor at Oregon Health & Science University and a leading researcher on hospice quality, having studied palliative and end-of-life care for more than two decades. Stepping in when families are unable to keep a patient comfortable isn’t just a gold standard, she said. Failure to do so can constitute “really poor quality hospice care.” If symptoms are too difficult to control, continuous in-person nursing care or admission to an inpatient unit could be necessary, she said. Death is “the one big sentinel event in that family and when it goes wrong, it’s really traumatic to them.”
AmeraCare declined to respond to specific questions about Ferdinand’s care.
During the first couple of months of the pandemic in New Orleans, hospice companies faced many of the same pressures as hospitals, workers told ProPublica. A hospice employee from AmeraCare, who spoke on the condition of anonymity, said that in-person visits were reduced to one per week, unless death was imminent. “If we could prevent going out and doing telehealth instead, like a patient not knowing the type of medication, the side effects, what it does, we could direct it on the phone,” they said. In Ferdinand’s hospice records, an AmeraCare staff member noted that the company was limiting skilled nursing visits and that they’d halted certified nursing assistant visits.
Taking the pandemic pressures into account, in late March, the Centers for Medicare and Medicaid Services
scaled back hospice regulatory requirements, allowing telehealth to replace face-to-face visits, if feasible and appropriate. CMS also dropped the requirement of having a nurse conduct an on-site hospice visit at least once every two weeks, allowing less qualified aides to provide care instead.
A nurse who worked at Compassus, the company that took care of Sarah Johnson, also said that their company limited visits. “We had decreased the amount of time that we go to the homes to once every two weeks unless they needed a nurse,” said the worker, who requested anonymity. “The patients had to really need a nurse. … None of us wanted to go in a house with a COVID patient since there is no control over how clean the surroundings would be. ... But we had to if we had to.”
Dana Coleman, a spokesperson for Compassus, told ProPublica that they equipped their workers with PPE, trained them on safety protocols and utilized virtual visits as permitted by CMS. She also said that additional staff members were deployed to New Orleans to maintain visit frequencies during the pandemic, and that nurse visits were not limited to once every two weeks.
Dr. Kai Romero, an emergency medicine doctor and the chief medical officer of Hospice by the Bay in Northern California, told ProPublica that they wouldn’t take on a COVID-19 hospice case unless there were adequate safety and infection control measures in place for family caretakers.
“In March and April, there wasn’t enough [PPE] for our own staff,” she said, adding that they ultimately needed to rely on the University of California, San Francisco, to help track down protective gear, such as masks for staff and family caretakers. “The considerations around who was going home on hospice, what supplies they’re given or can get access to, how that’s determined, is an extremely thoughtful process and if those don’t line up, at least here in San Francisco, we don’t admit them to home-based hospice.”
Ochsner did not respond to ProPublica’s questions about how it vetted hospice companies to see how prepared they were to handle the infectious disease, nor did they comment on the family caretakers who subsequently contracted the virus.
Before Johnson came home from the hospital, Compassus delivered a bed, oxygen tanks and morphine, and trained the family on how to administer the painkiller. “They tried to explain how to take care of her,” Lavalais said, “but it was hard to remember.”
Like the Ferdinands, Johnson’s family received no PPE. Lavalais, who is high risk with diabetes and hypertension, was deeply concerned. When he asked the company for masks, he received a box of gloves. Though difficult to find, the family tracked down a few surgical masks from a store, which was selling them for $5 apiece.
“Consistent with industry practices, we do not provide family caregivers with PPE as a matter of course,” said Coleman. “Given that many caregivers, friends, family, clergy, church members, neighbors, etc., may enter the home of a patient at any point during their time in hospice care, it is not possible for any provider to supply PPE for all possible visitors/exposures.”
Coleman pointed to CMS’s
guidance for hospice agencies during the pandemic, which says they should not be penalized for not providing PPE “if they are having difficulty obtaining these supplies for reasons outside of their control.”
The guidance also says “we do expect providers/suppliers to take actions to mitigate any resource shortages and show they are taking all appropriate steps to obtain the necessary supplies as soon as possible.”
When Johnson arrived, she seemed to have improved. She was alert, conversing with her children and even eating a little food. She told her son that when she regained her health, she wanted to visit her childhood home, a small shotgun house in the Seventh Ward. She wasn’t in pain, so he decided to not give her morphine and hoped that she might even recover before he would have to.
A hospice nurse checked in on Johnson the first two days she was home, said Lavalais and his brother, Michael. They assumed the daily visits would continue. But over the next 11 days, hospice workers came only two more times, they said. In contrast, a recent study analyzed data from a national, for-profit hospice company and found that, in normal times, home hospice patients
receive an average of about 7 visits per week from hospice workers, totaling about 9 hours of care time. Even in the pandemic, Teno said that in-person visits are important. “You should have PPE and you should be able to go in there and see the patient,” she said.
Coleman said that Compassus employees are available 24/7 for “emergent” calls or visits if a sudden need arises. While Compassus did not answer ProPublica’s questions about how many face-to-face visits were made to patients, Coleman said that if you include “virtual visits,” its patients were contacted four to fives times per week on average during the pandemic.
Johnson remained isolated in her bedroom, the door cracked open so her sons could check on her. She grew weaker. A little over a week into her stay at home, Lavalais watched her struggle to swallow as she tried to drink. It sounded “like a piece of steel was stuck in her throat,” he said, “and the water couldn’t go through.”
When she’d shown signs of this problem at West Bank, a speech therapist evaluated her and gave careful recommendations on how to handle it in the hospital, like thickening liquids to make them easier for Johnson to drink. No one told the family about the issue.
Lavalais called the hospice company; he says he was told to stop giving his mother food and water, which is not an unusual practice for hospice patients close to death. He was also told to increase the morphine. Lavalais asked if she should be readmitted to the hospital. “The hospice nurse said, ‘They won’t be able to do anything for her, but I can’t tell you what to do,’” he said.
When Johnson asked her son for water, saying she was thirsty, Lavalais didn’t know what to do. “I couldn’t give her anything,” he said. “I felt terrible.” He and his brother said that as Johnson worsened during her final three days, no hospice nurse visited.
Coleman said patients always have the right to revoke hospice care and seek more aggressive or curative care at a hospital; under Medicare, hospice patients can also go to the hospital if they have “uncontrolled pain that cannot be managed at home.” Compassus declined to answer specific questions about Johnson, despite having a waiver from her son permitting them to speak about her care.
“When someone is in the dying process, they develop a constellation of more symptoms,” said Teno, adding that when death is imminent, symptoms can be hard to control. “We know that when visits don’t occur in the last few days of life, it’s very stressful for the family.” These visits are so critical that the federal government
uses them to evaluate hospice quality.
When Johnson’s children moved her, “she would moan and groan in pain,” Lavalais said. “I was overwhelmed. I didn’t feel comfortable.”
On the morning of May 3, Lavalais walked into his mother’s room to check in on her and saw that she wasn’t breathing. Thirteen days after coming home from the hospital, she had passed. “I thought she’d be in good hands,” her son said. “I know she suffered.”